Documente Academic
Documente Profesional
Documente Cultură
3.5small Intestines (Licup) - Pacis PDF
Încărcat de
Kirchner PatrollaTitlu original
Drepturi de autor
Formate disponibile
Partajați acest document
Partajați sau inserați document
Vi se pare util acest document?
Este necorespunzător acest conținut?
Raportați acest documentDrepturi de autor:
Formate disponibile
3.5small Intestines (Licup) - Pacis PDF
Încărcat de
Kirchner PatrollaDrepturi de autor:
Formate disponibile
[SURGERY] SMALL INTESTINES – DR.
LICUP
SMALL INTESTINES
Dr. Licup
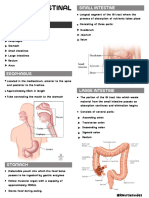
SMALL INTESTINES
Site of nutrient digestion and absorption
Largest reservoir of immunologically active and hormone-
producing cells
Largest organ of immune and endocrine system
4 Parts of the Duodenum:
It produces 75% of our body’s immune system.
1st Part: Superior
Diseases are relatively infrequent 2nd Part: Descending
- Importance: Major duodenal papilla
Except for Small Bowel Obstruction (SBO) 3rd Part: Inferior/Horizontal
4th Part: Ascending
Ligament of Treitz = separates the duodenum from
GROSS ANATOMY the jejunum
Tubular structure extending from pylorus to cecum Above the ligament = Duodenum
Measures about 4-6m Below the ligament = Jejunum
3 Segments:
Duodenum
Jejunum JEJUNUM AND ILEUM
Ileum Within the peritoneal cavity
Since they are within the peritoneal cavity, they
need an attachment Attached to the mesentery
Broad-based mesentery (blood supply)
Proximal 40% Jejunum
Distal 60% Ileum
PLICAE CIRCULARS OR VALVULAE CONNIVENTES
Duodenum: First part of the small intestines
Jejunum: Upper 2/5
Ileum: Lower 3/5 Mucosal folds, visible upon gross inspection
Visible radiographically
If your patient got stabbed in the left upper Distinction between small intestine and colon
quadrant, the most likely injured part of the small Colon = Haustrations
bowel is the jejunum. Small Intestines = Plicae Circularis
If your patient got stabbed in the right lower More prominent in the proximal intestine
quadrant, the most likely injured part of the small
bowel is the ileum. PROXIMAL INTESTINES
There is no distinguishing landmark that separate the
DUODENUM jejunum from ileum, but we could still differentiate
Most proximal segment jejunum from ileum by the following features:
Retroperitoneum
Demarcated from the Larger circumference
Stomach by the pylorus Thicker walls
Jejunum by the ligament of Treitz Less fatty mesentery
Blood Supply: Celiac and Superior Mesenteric Arteries Longer vasa recta
LEA THERESE R. PACIS 1
[SURGERY] SMALL INTESTINES – DR. LICUP
SUMMARY Surgeons sometimes do resection of the small
JEJUNUM ILEUM intestines and anastomose it. When they
Larger circumference Small circumference anastomose it, they use the strongest layer. By
Thicker walls Thinner wall anastomosing the strongest layer, you are going
Less fatty mesentery More fatty mesentery to lessen the possibility of anastomotic leak.
Longer vasa recta Shorter vasa recta
Muscularis externa
Serosa
PEYER’S PATCHES
Aggregates of lymphoid follicles PHYSIOLOGY
Located mainly in the ileum DIGESTION AND ABSORPTION
Intestinal epithelium Absorption and secretion occur
Lymphoid follicles in the mesentery Mesenteric
Nodes Villi Main absorptive structures
Jejunum Where 95% of water is absorbed, as well
as nutrients
SUPERIOR MESENTERIC ARTERY Ileum Absorption and digestion into bile acid
Distal duodenum, jejunum, ileum
Solutes traverse by active or passive mechanisms:
SUPERIOR MESENTERIC VEIN (Drainage) Passive Transport of Solutes
- Diffusion or convection
Small intestines drains to the Superior Mesenteric - Driven by existing electrochemical gradients
Vein Portal Vein Liver - Occurs through either transcellular or paracellular
pathways (between cells through the tight junctions)
Active Transport
LYMPH NODES - Energy-dependent net transfer of solutes in absence or
Mesenteric Lymph Nodes Cistern Chyli Thoracic Duct against an electrochemical gradient
Left Subclavian Vein - Occurs through transcellular pathways (through the
cell)
INNERVATION
Parasympathetic and Sympathetic Supplies form Vagus and WATER AND ELECTROLYTES
Splanchnic Nerve 8-9L of fluid/day
WALL HAS FOUR DISTINCT LAYERS Approximately 2L comes from your oral intake
The rest of it comes from salivary, gastric, biliary,
pancreatic and intestinal secretions
Normally 80% absorbed
1.5L enters the colon
If less than 1.5L enters the colon Constipation
CARBOHYDRATE DIGESTION AND ABSORPTION
45% of energy consumption in average Western diet
Pancreatic amylase is the major enzyme of starch digestion,
although salivary amylase initiates the process.
Duodenum/Upper Jejunum Absorption of
Mucosa monosaccharides
Epithelium: enterocytes (absorptive), goblet cells, paneth 10% dietary starch passes unabsorbed into the colon
cells, enterochromaffin cells Fiber – indigestible Increases osmotic load to distal small
Lamina Propia: containing Payer’s patches bowel and Colon Increases stool mass
Water and nutrient absorption across the mucosa
Submucosa For a constipated person, aside from increasing their
Strongest layer/connective tissues water intake, to increase their stool mass, you should
Meissner’s plexus also advise them to take high fiber diet.
LEA THERESE R. PACIS 2
[SURGERY] SMALL INTESTINES – DR. LICUP
PROTEIN DIGESTION AND ABSORPTION Included in this epithelial defense are your:
10-15% of energy consumption IgA
For surgical patients, they need protein to hasten and Mucins
increase their wound healing process. Impermeability of the brush borders
In the hospital, if they require the patient to have a Anti-microbial peptides (defensins)
high protein diet, they usually give egg whites. Gut-associated lymphoid tissues (GALT)
Protein is denatured and partially digested STOMACH Gut-associated lymphoid tissue (GALT)
(Pepsin) Contains over 70% of the body’s immune cells
Inductive sites Peyer’s patches mesenteric lymph
Pancreatic enzymes digest proteins to form free amino acids
nodes, smaller isolated lymphoid follicles
and oligopeptides
Digestion continues in the duodenum Pancreatic How do you stimulate the GALT?
peptidase By stimulating the small intestines through feeding
80% of protein absorption occur in the proximal That is why for surgical patients, they are
100cm of the jejunum advised to eat at the soonest possible time to be
able to stimulate the body’s immune system
FAT DIGESTION AND ABSORPTION IgA
40% Fat Prevent the entry of microbes through the epithelium
Promote excretion of antigens or microbes that have
Over 95% of dietary fat is in the form of long chain
already penetrated into the lamina propria
triglycerides
Remainder includes phospholipids such as lecithin, fatty
MOTILITY
acids, cholesterol, and fat-soluble vitamins
Contractions of the muscularis propria are responsible for
94% of the ingested fats are absorbed in the duodenum and
small intestinal peristalsis
proximal jejunum
Contraction of the outer longitudinal muscle layer results in
Duodenum and proximal jejunum Presence of bile bowel shortening
Bile comes of the 2nd portion of the duodenum
Used for fat emulsification Outer Longitudinal Shortens
Inner Circular Narrows
VITAMIN AND MINERAL ABSORPTION Several distinctive patterns of muscularis propria activity
Dietary Vitamin B12 (cobalamin) complexes with intrinsic Include ascending excitation and descending inhibition
factor (mucoprotein secreted by gastric parietal cells) Muscular contraction occurs proximal to a stimulus
Complex dissociates at the surface of cells in the distal ileum Muscular relaxation occurs distal to the stimulus
where B12 enters the cells
In the stomach: Vitamin B12 + Intrinsic Factor Go
to the ileum Dissociate Absorbed into the
circulation
If you have a patient who underwent gastric
resection/gastric bypass There would be a problem
with the absorption of Vitamin B12 Give them
vitamin B12 replacement
Proximally, there is shortening and narrowing;
Preoperatively if there is no identified vitamin and Distally, there is lengthening and widening That is
mineral deficiencies in you patient You do not have why peristalsis in ONE WAY
to supplement them
Fat soluble vitamins (ADEK) Impaired absorption in
ENDOCRINE FUNCTION
absence of BILE
SI largest hormone-producing organ in the body
Over 30 peptide hormone genes
BARRIER AND IMMUNE FACTORS
Histamine and dopamine, eicosanoids with hormone-like
The epithelium of the small intestine identifies pathogen
activities are produced in the small intestines
from harmless antigen
Prevents invasion from these pathogens
LEA THERESE R. PACIS 3
[SURGERY] SMALL INTESTINES – DR. LICUP
Table 28-2 Representative Regulatory Peptides Produced in Obstructing lesion categorized as:
the Small Intestine 1. Intraluminal (e.g., foreign bodies, gallstones or
meconium)
Intraluminal = obstruction within the lumen of the
small intestine
2. Intramural (e.g., tumors, Crohn’s disease-associated
inflammatory structures)
Intramural = obstruction within the walls of the
small intestine
Octreotide
3. Extrinsic (e.g., adhesions, hernias, or carcinomatosis)
Long acting analogue of somatostatin neuroendocrine
tumors (e.g., carcinoid syndrome) Extrinsic = obstruction that results from outside the
Postgastrectomy dumping syndrome, enterocutaneous small intestine
fistulas
Acute hemorrhage due to esophageal varices Intra-abdominal Adhesions
Cholecystokinin (CCK) – cells of proximal intestines Post-operative adhesions
Secretin – S cells of proximal intestines Up to 75% of the cases of small obstruction
Motilin – M cells of proximal intestines
Somatostatin – D cells throughout the gut If a patient comes to you with small bowel
obstruction, the first thing that you should know is
INTESTINAL ADAPTATION if she/he has had previous abdominal surgery
Capacity to adapt Physiologic and pathologic conditions
Less prevalent etiologies
Massive small bowel resection (Postresection intestinal
Hernias
adaption)
Malignant bowel obstruction
Within a few hours after bowel resection Epithelial
Crohn’s disease
cellular hyperplasia Villi lengthen, absorptive surface
Cancer-related SBO Extrinsic compression or invasion
area increase, digestive and absorptive functions improve
Few are due to primary small bowel tumors
Mechanisms under active investigation
Table 28-3 Most Commonly Encountered Etiologies of SBO
Jejunal resection generally is better tolerated
Ileum shows better capacity to compensate
There is a higher chance that you will have Short
Bowel Syndrome if you cut on the ileum because
jejunum does not compensate as well as the ileum.
Short bowel syndrome
When you cut the intestine Villi will lengthen
If the villi did not compensate You will have
malabsorption Short Bowel Syndrome
SMALL BOWEL OBSTRUCTION
Most disease of the small bowel are not common If
you were able to see one, most likely it is a Small Bowel
Obstruction
75% of SBO cases are secondary to post-operative
adhesions
LEA THERESE R. PACIS 4
[SURGERY] SMALL INTESTINES – DR. LICUP
Congenital Abnormalities Ideally, surgical management must be minimally
Intestinal malrotation invasive or laparoscopic adhesiolysis To prevent
Midgut volvulus recurrence of adhesions
Congenital bands
Complete Small Bowel Obstruction
PATHOPHYSIOLOGY Closed Loop Obstruction
Obstruction Gas and fluid accumulate proximal Surgical emergency!
Intestinal activity increases The colicky pain and the A segment of intestine is obstructed both proximally and
diarrhea distally Leading to a rapid rise in luminal pressure
Rapid progression to strangulation Ischemia, necrosis,
Initially, what the small intestines will do is become perforation
hyperactive To remove/bypass the obstruction
Stop Hyperactive Stop, and so on Colicky pain
and diarrhea
Accumulation of fluid is secondary to intake. If the
patient does not have any intake, it may be due to
salivary secretion, biliary secretion and gastric
secretions.
Most of the gas Swallowed air/within the intestine
Bowel distends Intraluminal and intramural pressures rise
Initially there is hyperactive bowel sounds Later
there will be hypoactive or no bowel sounds
Intestinal motility Reduced with fewer contractions
Obstruction Luminal flora of the bowel (sterile)
Infected
Translocation of these bacteria to regional lymph nodes (+) Air-fluid leveling
Stepladder sign Sign of SBO
Inside the distended bowel, the intestinal content
must be sterile But since it is not drained, it
becomes infected Then that infection inside the CLINICAL PRESENTATION
bowel will go to the mesenteric nodes = Translocation Symptoms: Colicky abdominal pain, nausea, vomiting and
of bacteria obstipation
From the nodes, it will disseminate to the different Vomiting with proximal obstructions than distal
parts of the body That is why small bowel Character of vomitus is important
obstruction, antibiotics are usually given To
prevent translocation of bacteria Fecaloid Distal Obstruction
Not bile-stained Obstruction around the 1st or
Strangulated bowel obstruction Intramural pressure 2nd portion of intestines
increases, microvascular perfusion is impaired Ischemia Bile stained Obstruction on the 3rd portion
Necrosis onwards
Distended bowel Impingement of blood vessels Continued passage of flatus and/or stool beyond 6-12
Compromised blood circulation Ischemia hours
Gangrene Necrosis Perforation Signs: Abdominal distention (pronounce if ileum)
Bowel sounds may be hyperactive initially
TYPES SBO ILEUS
Partial Small Bowel Obstruction Hyperactive bowel Hypoactive from the
Only a portion is occluded sound initially, then start till the end
Allowing passage of some gas and fluid later hypoactive
Usually treated medically If it already happened 3
Laboratory Findings
times Undergo surgery
Intravascular volume depletion
LEA THERESE R. PACIS 5
[SURGERY] SMALL INTESTINES – DR. LICUP
Hemoconcentration, electrolyte abnormality 2. Obstruction occurring in the early postoperative period
Strangulated 3. Intestinal obstruction due to Crohn’s disease
Severe abdominal pain 4. Carcinomatosis
Jejunum Most likely: Left upper quadrant pain ILEUS
Ileum Most likely: Right lower quadrant pain Impaired intestinal motility
Signs and symptoms of intestinal obstruction in the absence
Tachycardia
of a lesion-causing mechanical obstruction
Localized abdominal tenderness
Ileus is a temporary motility disorder that is reversed if
Fever
corrected
Marked leukocytosis
Table 28-4: Common Etiologies
Diagnosis
History & PE
History of post-abdominal surgery
Hernias
Stool checked for gross of occult blood Intestinal
strangulation
CT scanning is 80-90% sensitive and 70-90% specific
Closed-loop Obstruction U-shaped or C-shaped dilated
bowel loop
Abdominal series consist of:
- Radiograph: Upright/supine position
- CXR (Upright)
To know if there is pneumoperitoneum Signify
perforation
Most likely there is a perforation of the
stomach or duodenum or perforation of the
colon
- Triad of dilated small bowel loops (> 3 cm in diameter)
air-fluid levels, paucity of air in the colon
Sensitivity x-ray from 70-80%
THERAPY
Most Common: Electrolyte imbalance
6 Ns in Treating SBO: Hypokalemia
NPO (Nothing per orem)
Intestinal motility return to normal within first 24 hours
NSS IV fluid hydration
after laparotomy
NGT (Nasogastric tube)
Gastric and colonic motility returning to normal by 48 hours
aNtacids
and 3-5 days respectively
aNtibiotic
iNdwelling Folley Catheter (IFC) Intra-abdominal abscesses or electrolyte abnormalities
Post-operative: Consider intra-abdominal abscess
Fluid resuscitation Isotonic fluid
Drain the abscess
IFC to monitor urine output
Percutaneous (UTZ-guided) = Single
Central-venous or pulmonary-artery catheter monitoring
Open-technique = Multiple or near the major blood
Broad-spectrum antibiotics (bacterial translocation)
vessels
NG tube Decompression
Complete Small Bowel Obstruction
In general, the treatment is surgery CLINICAL PRESENTATION
Advocated non-operative approaches if closed loop Inability to tolerate liquids and solids by mouth
obstruction is ruled out Nausea
Conservative Therapy Lack of flatus or bowel movements
1. Partial small bowel obstruction Vomiting and abdominal distention
LEA THERESE R. PACIS 6
[SURGERY] SMALL INTESTINES – DR. LICUP
Bowel sounds are characteristically diminished or absent Therapy No curative therapies
Goal of treatment is to palliate symptoms
DIAGNOSIS Medical therapy is used to induce and maintain disease
Ileus beyond 3-5 days postoperatively or occurs in the remission
absence of abdominal surgery, diagnostic evaluation is Surgery is reserved for specific indications
needed Nutritional support enteral regimens or parenteral
Opiates impair intestinal motility nutrition
Serum electrolytes Table 28-8: Indications for Surgical Intervention in
Abdominal radiographs/CT scan Crohn’s Disease
- Acute onset of severe disease
THERAPY - Failure of medical therapy
Limiting oral intake - Obstruction
Correcting the underlying inciting factor - Hemorrhage
Vomiting or abdominal distention are prominent NGT
IV fluid and electrolytes
TPN, early ambulation
Administration of NSAIDS such as ketorolac
Reduction in opioid dosing
Table 28-6 summarizes some of the measures used to
minimize postoperative ileus
INTESTINAL FISTULA
Fistula Abnormal communication between two
epithelialized surfaces
Internal Fistula (e.g., enterocolonic fistula or colovesicular
CROHN’S DISEASE
fistula)
Chronic, idiopathic transmural, inflammatory disease
Propensity to affect to distal ileum Non-resectable Cecal Tumor Fluid from the ileum
Any part can be involved cannot go to the ascending colon What you can do
Eastern European Jewish population are at 2-4 fold higher is to create an internal fistula Connect the ileum to
risk the ascending colon and make an enterocolonic
Slightly more prevalent in females than in males fistula, bypassing the cecal tumor
Third decade
Higher socioeconomic status External Fistula (e.g., enterocutaneous fistula or
Breastfeeding to be protective rectovaginal fistula)
More prevalent among smokers
You can also make an external fistula
enterocutaneous fistula (ileostomy) Ileum to the
CLINICAL PRESENTATION
skin
Abdominal pain, diarrhea, weight loss
Depends on which segment of the GIT is affected Low-output fistulas Drain less than 200mL of fluid per day
Patients with Crohn’s disease can be classified by their
predominant clinical manifestation as having primarily Low-output fistulas are treated medically
a. Fibrostenotic disease Lessen passage of fluid Give TPN, low-residue
b. Fistulizing disease, and diet (colocutaneous fistula), elemental diet
c. Aggressive inflammatory disease (enterocutaneous fistula)
Affects the small bowel in 80% of cases, and colon alone 20%
LEA THERESE R. PACIS 7
[SURGERY] SMALL INTESTINES – DR. LICUP
High-output fistulas Drain more than 500mL of fluid per CLINICAL PRESENTATION
day Most are asymptomatic until they become large
Partial SBO
High-output fistulas are treated surgically unless you Associated signs and symptoms of crampy abdominal pain
can convert it to a low-output fistula and distention, N/V
Give Octerotide or Somatostatin Decrease output
Obstruction Luminal narrowing or intussusceptions
Iatrogenic, post-operative complications, Crohn’s disease or Hemorrhage, indolent, is 2nd most common presentation
cancer PE may be unrevealing
Jaundice secondary to biliary obstruction or hepatic
DIAGNOSIS metastasis (if duodenal area is affected there will be a
CT painless jaundice)
Intra-abdominal abscess should be sought and drained Cachexia, hepatomegaly, and ascites may be present with
percutaneously advanced disease
Small bowel series Adenocarcinomas, as well as adenomas are most common
Fistulogram in duodenum
THERAPY THERAPY
Treatment proceed sequence of steps Benign symptomatic neoplasm Surgically resected or
1. Stabilization Fluid and electrolyte, nutrition is provided, removed endoscopically
antibiotics, drainage, ostomy appliances or fistula drains EGD Lesions should be biopsied
2. Investigation Diagnosis In general:
3. Decision Available treatment <1cm Endoscopic polypectomy
Timing of Surgical Intervention Lesions > 2cm Removed surgically
2-3 months of conservative therapy Surgical Options:
90% of fistulas that are going to close Transduodenal polypectomy and segmental duodenal
If fistulas fails to resolve during this period Surgery resection
Pancreaticoduocenectomy (Whipples)
SMALL BOWEL NEOPLASM The surgical therapy of jejuna and ileal malignancies
(NOT DISCUSSED BUT NEEDS TO BE STUDIED) Wide local resection
Adenomas, most common benign neoplasm Adenocarcinomas Wide excision of corresponding
Other benign tumors include fibromas, lipomas, mesentery
hemangiomas, lymphangiomas, and neurofibromas Locally advanced or metastatic disease Palliative
Lesions are most frequently encountered in the duodenum intestinal resection or bypass
during EGD
Benign neoplasms account for 30 to 50% of small bowel RADIATION ENTERITIS
(NOT DISCUSSED BUT NEEDS TO BE STUDIED)
tumors and include adenomas, lipomas, hemartomas, and
hemangiomas. Radiation-induced injury to the small intestine
Primary small bowel cancers are rare 2 distinct syndromes: Acute & Chronic Radiation Enteritis
Adenocarcinomas comprise 35-50% of all cases, carcinoid Acute Radiation Enteritis Transient, in approximately
tumors comprising 20-40% of cases, and lymphomas 10-15% 75%
of cases Chronic Radiation Enteritis In 5-15%
GIT STROMAL TUMORS (GISTS) THERAPY
Most common mesenchymal tumors Most cases of acute radiation enteritis are self-limited
Supportive therapy
Comprise up to 15% of small bowel malignancies
Rarely reduction in or cessation of radiation therapy
Formerly classified as leiomyomas, leiomyosarcomas, and
Surgery only done if needed Difficult with high morbidity
smooth muscle tumors
Limited resection of diseased intestine
Frequent site for metastases
5th or 6th decade of life
MECKEL’S DIVERTICULUM
Reported Risk Factors (NOT DISCUSSED BUT NEEDS TO BE STUDIED)
Consumption of red meat Most prevalent congenital anomaly of GIT
Ingestion of smoked or cured foods 2% of the general population
Crohn’s disease 3:2 M:F prevalence ratio
Celiac sprue True Diverticula Contains all layers of normal intestine
LEA THERESE R. PACIS 8
[SURGERY] SMALL INTESTINES – DR. LICUP
Usually found in ileum within 100cm of ileocecal valve INTUSSUSCEPTION
60% contain hetertopic mucosa >60% gastric mucosa (NOT DISCUSSED BUT NEEDS TO BE STUDIED)
One segment of the intestine becomes drawn into the lumen
of the proximal segment of the bowel
RULE OF TWO
Usually in the pediatric population
2% prevalence
Cecum intussuscepted into the ileum (ileocolic
2:1 female preponderence
intussusceptions)
Location 2 ft proximal to the ileocecal valve in adults
Treated nonsurgically by radiologic reduction (barium
½ of those who are symptomatic are under 2yo
enema increases pressure which will force the
intussuception to resolve)
CLINICAL PRESENTATION
Adult intussusceptions are less common
Asymptomatic
Malignant lead point in ½ of cases
Most common symptoms are bleeding, intestinal
Intermittent abdominal pain and S/S of bowel obstruction
obstruction, and diverticulitis
CT scan “target sign” may be seen
Most common disease associated with Meckel’s
diverticulum is appendicitis Treatment is surgical resection of the involved segment and
the lead point
THERAPY
PNEUMATOSIS INTESTINALIS
Diverticulotomy with removal of associated bands (NOT DISCUSSED BUT NEEDS TO BE STUDIED)
Bleeding, tumor, perforation Segmental resection Presence of gas within the bowel wall
Incidentally found (asymptomatic) Common in the jejunum
NOT a disease but merely a sign
ACQUIRED DIVERTICULA Association with bowel ischemia and infarction
(NOT DISCUSSED BUT NEEDS TO BE STUDIED)
False Diverticula Lack muscularis layer of the SI Necessitate emergent surgical intervention
More common in the duodenum, near the ampulla of vater
SHORT BOWEL SYNDROME
Periampullary, juxtapapillary, or peri-Vaterian diverticula (NOT DISCUSSED BUT NEEDS TO BE STUDIED)
Jejunoileal diverticula Acquired diverticula in the jejunum Extent of resection is great enough
or ileum Defined as the presence of <200cm of residual small bowel
Functional definition, insufficient intestinal absorptive
CLINICAL PRESENTATION capacity results in the clinical manifestations of diarrhea,
Asymptomatic dehydration, and malnutrition, is more broadly applicable
Intestinal obstruction, diverticulitis, bleeding, abdominal In adults, acute mesenteric ischemia, malignancy, and
pain Crohn’s disease
Periampullary duodenal diverticula In pediatric patient Intestinal atresias, volvulus, and NEC
Treatment: TPN, intestinal transplant, or intestinal
THERAPY transplant
Asymptomatic None
Bacterial overgrowth Antibiotics
Bleeding and diverticulitis Segmental intestinal resection Source: Recordings + Old Book Trans (2011) + Schwartz's
Diverticulotomy Bleeding and obstruction related to Principles of Surgery, 10th Edition
lateral duodenal diverticula
SMALL BOWEL PERFORATIONS
(NOT DISCUSSED BUT NEEDS TO BE STUDIED)
Before 1980s, duodenal perforation was due to peptic ulcer
Iatrogenic injury GI endoscopy is the most common
Other etiologies
infections
Crohn’s disease
Ischemia
Drugs (Potassium and NSAIDs)
Radiation induced
Meckel’s and Acquired Diverticulitis
Neoplasm
Foreign bodies
LEA THERESE R. PACIS 9
S-ar putea să vă placă și
- Intestinal Diseases, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsDe la EverandIntestinal Diseases, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsÎncă nu există evaluări
- NCM107 PediatricsDocument11 paginiNCM107 PediatricsKM PanganibanÎncă nu există evaluări
- AppendicitisDocument132 paginiAppendicitisPauLa Cheneree Peña ÜÎncă nu există evaluări
- Surgey of The Small Intestine in Dogs and Cats Part 1Document6 paginiSurgey of The Small Intestine in Dogs and Cats Part 1Luis Espinola UribeÎncă nu există evaluări
- MS GiDocument35 paginiMS GiFrances GabbuatÎncă nu există evaluări
- Ana SGD 15Document67 paginiAna SGD 15Bea ManzanoÎncă nu există evaluări
- Etiologi Dan Patofisiologi Bedah DigestifDocument46 paginiEtiologi Dan Patofisiologi Bedah DigestifNurul HidayatiÎncă nu există evaluări
- The Small Intestine - Duodenum - Jejunum - Ileum - TeachMeAnatomyDocument4 paginiThe Small Intestine - Duodenum - Jejunum - Ileum - TeachMeAnatomyFelix Oriono100% (1)
- Large Intestine PIMSR-Dr - Gosai 2022Document40 paginiLarge Intestine PIMSR-Dr - Gosai 2022Dr.B.B.GosaiÎncă nu există evaluări
- Anatomy SGD (Lower GIT)Document7 paginiAnatomy SGD (Lower GIT)staezyevans100% (1)
- The Digestive System in 40 CharactersDocument4 paginiThe Digestive System in 40 CharactersSofronio OmboyÎncă nu există evaluări
- M1207 GIT E2 ForegutDocument29 paginiM1207 GIT E2 Foregutkavinduherath2000Încă nu există evaluări
- Small intestinal surgery principlesDocument12 paginiSmall intestinal surgery principlesSara ConnorÎncă nu există evaluări
- Jejunum IleumDocument55 paginiJejunum IleumDitas ChuÎncă nu există evaluări
- The Concise Medical Encyclopedia - AnnDocument520 paginiThe Concise Medical Encyclopedia - AnnANIL KUMARÎncă nu există evaluări
- Repaso 5 ANATOMY JEJUNUM LJ ILEUM L0 COLONDocument4 paginiRepaso 5 ANATOMY JEJUNUM LJ ILEUM L0 COLONAngelitza AlmodóvarÎncă nu există evaluări
- Anatomy, Histology, Embryology, and DevelopmentalDocument41 paginiAnatomy, Histology, Embryology, and DevelopmentalNikhilesh YandamuriÎncă nu există evaluări
- SB TumorsDocument34 paginiSB TumorsAsdawi B. DicritanÎncă nu există evaluări
- Jejunal and Ileal AtresiasDocument37 paginiJejunal and Ileal AtresiasABDUL RAHIM UMAR FAROUKÎncă nu există evaluări
- Anatomy of Lower Gastrointestinal TractDocument26 paginiAnatomy of Lower Gastrointestinal TractOmar Ali AyoubkhanÎncă nu există evaluări
- Gross Anatomy of The Digestive System Lecture Notes Lecture 2Document5 paginiGross Anatomy of The Digestive System Lecture Notes Lecture 2Lorelie AsisÎncă nu există evaluări
- The Small Intestine-1Document38 paginiThe Small Intestine-1ChiderahÎncă nu există evaluări
- Midterm Genana ReviewerDocument9 paginiMidterm Genana ReviewerNATALIE NICOLE GABASÎncă nu există evaluări
- A Look at The: Small IntestineDocument16 paginiA Look at The: Small IntestineSandra RubianoÎncă nu există evaluări
- Abdominal Wall, Omentum, Mesentery and Retroperitoneum DR AsepkyDocument33 paginiAbdominal Wall, Omentum, Mesentery and Retroperitoneum DR Asepkyafwan fajriÎncă nu există evaluări
- Peritoneum 2022Document86 paginiPeritoneum 2022Tayyib KhanÎncă nu există evaluări
- M1207: Gastrointestinal System Embryology Lecture 01: Dr. Sampath PaththinigeDocument30 paginiM1207: Gastrointestinal System Embryology Lecture 01: Dr. Sampath Paththinigekavinduherath2000Încă nu există evaluări
- Anatomy Small IntestineDocument1 paginăAnatomy Small IntestinetristineÎncă nu există evaluări
- Abdominal Cavity Anatomy ReviewDocument15 paginiAbdominal Cavity Anatomy ReviewCaperlac MarjorieÎncă nu există evaluări
- The Abdominal OrgansDocument56 paginiThe Abdominal OrgansAjeng FikihÎncă nu există evaluări
- Development of Alimentary System Part 1Document52 paginiDevelopment of Alimentary System Part 1Aarushi JainÎncă nu există evaluări
- Abdominal Cavity Anatomy and ApproachesDocument4 paginiAbdominal Cavity Anatomy and ApproachesAwais Usman MirzaÎncă nu există evaluări
- Bahan Pemicu 3 Gastrointestinal Ivan BuntaraDocument109 paginiBahan Pemicu 3 Gastrointestinal Ivan BuntaraMarco GunawanÎncă nu există evaluări
- 4Document9 pagini4Marielle Anne TuazonÎncă nu există evaluări
- Stomach, Duodenum, Pancreas, and Spleen AnatomyDocument4 paginiStomach, Duodenum, Pancreas, and Spleen AnatomyJoshua MandaweÎncă nu există evaluări
- m1207 Git E3 MidgutDocument24 paginim1207 Git E3 Midgutkavinduherath2000Încă nu există evaluări
- Lecture 12Document4 paginiLecture 12A-Naeem To'mah Al-sawaieÎncă nu există evaluări
- L6 - OmentumDocument12 paginiL6 - OmentumGoodone OneÎncă nu există evaluări
- Colon, Caecum & Appendix 2017Document67 paginiColon, Caecum & Appendix 2017yasrul izad0% (1)
- 4 Peritoneum PDFDocument64 pagini4 Peritoneum PDFN AÎncă nu există evaluări
- Digestive System: Abdominal QuadrantsDocument4 paginiDigestive System: Abdominal QuadrantsAngel Rose BrillanteÎncă nu există evaluări
- DIgestive System EmbDocument85 paginiDIgestive System EmbDanish GujjarÎncă nu există evaluări
- Development of GIT - IDocument69 paginiDevelopment of GIT - IAarushi JainÎncă nu există evaluări
- Anorectal DiseasesDocument21 paginiAnorectal DiseasesPurple Ivy GuarraÎncă nu există evaluări
- Esophagus AnatomyDocument5 paginiEsophagus AnatomyJinÎncă nu există evaluări
- Anatomy (Compatibility Mode)Document34 paginiAnatomy (Compatibility Mode)your babysurgeonÎncă nu există evaluări
- Radiology Examination For Tractus Digestivus Chairunnisa, Dr. SP - RadDocument100 paginiRadiology Examination For Tractus Digestivus Chairunnisa, Dr. SP - RadDiana OCtavinaÎncă nu există evaluări
- Gastro NotesDocument11 paginiGastro NotesMonica JubaneÎncă nu există evaluări
- Genitourinary and Reproductive Systems AnatomyDocument4 paginiGenitourinary and Reproductive Systems AnatomyLester AldridgeÎncă nu există evaluări
- Structure of Peritoneum: Where Does It Come From?Document40 paginiStructure of Peritoneum: Where Does It Come From?Ryan GosserÎncă nu există evaluări
- HerniaDocument106 paginiHerniaDr-Mohammad Ali-Fayiz Al TamimiÎncă nu există evaluări
- COLON ANATOMY AND SURGERYDocument37 paginiCOLON ANATOMY AND SURGERYDjan Kurvie ValencerinaÎncă nu există evaluări
- Physiology of Lower GI TractDocument180 paginiPhysiology of Lower GI TractIcarus WingsÎncă nu există evaluări
- Anatomy and Physiology of RectumDocument5 paginiAnatomy and Physiology of RectumDoreen Claire M. WallangÎncă nu există evaluări
- Ans of AbdomenDocument69 paginiAns of Abdomenpasha100% (1)
- Peritoneum and Gastro-Intestinal TractDocument108 paginiPeritoneum and Gastro-Intestinal TractKAYISIRE EMERYÎncă nu există evaluări
- Digestive System Breakdown and AbsorptionDocument9 paginiDigestive System Breakdown and AbsorptionTana OquendoÎncă nu există evaluări
- Reviewer For Zoology LabDocument18 paginiReviewer For Zoology LabayeyedumpÎncă nu există evaluări
- 1234 StomachDocument6 pagini1234 StomachShubham NainwayaÎncă nu există evaluări
- Peritoneum and Peritoneal CavityDocument26 paginiPeritoneum and Peritoneal CavitytuhinsinghÎncă nu există evaluări
- Orthopedics Part 03 PDFDocument5 paginiOrthopedics Part 03 PDFKirchner PatrollaÎncă nu există evaluări
- Spinal Fractures Assessment and ManagementDocument10 paginiSpinal Fractures Assessment and ManagementKirchner PatrollaÎncă nu există evaluări
- Surgery 3.02 Small Intestines - Dr. HawDocument21 paginiSurgery 3.02 Small Intestines - Dr. HawKirchner PatrollaÎncă nu există evaluări
- Learner Enrollment FormDocument2 paginiLearner Enrollment Formnicole marqueses93% (71)
- Pages 1245 - 1255 (Radiation Enteritis To Short Bowel Syndrome) PDFDocument4 paginiPages 1245 - 1255 (Radiation Enteritis To Short Bowel Syndrome) PDFKirchner PatrollaÎncă nu există evaluări
- Chapter 25 p.1060-1075 PDFDocument16 paginiChapter 25 p.1060-1075 PDFKirchner PatrollaÎncă nu există evaluări
- Pages 1028-1043 (Video and Cineradiography - Outcome After Fundoplication) PDFDocument5 paginiPages 1028-1043 (Video and Cineradiography - Outcome After Fundoplication) PDFKirchner PatrollaÎncă nu există evaluări
- Pages 1028-1043 (Video and Cineradiography - Outcome After Fundoplication) PDFDocument5 paginiPages 1028-1043 (Video and Cineradiography - Outcome After Fundoplication) PDFKirchner PatrollaÎncă nu există evaluări
- Pages 1219-1233 (Small Intestine Anatomy - Bowel Obstruction) PDFDocument5 paginiPages 1219-1233 (Small Intestine Anatomy - Bowel Obstruction) PDFKirchner PatrollaÎncă nu există evaluări
- Pages 1245 - 1255 (Radiation Enteritis To Short Bowel Syndrome) PDFDocument4 paginiPages 1245 - 1255 (Radiation Enteritis To Short Bowel Syndrome) PDFKirchner PatrollaÎncă nu există evaluări
- 4bi1 2b Que 20230117Document20 pagini4bi1 2b Que 20230117ah6643242Încă nu există evaluări
- Immuno OncologyDocument4 paginiImmuno OncologydanieleÎncă nu există evaluări
- Human Body Structure from Cells to TissuesDocument44 paginiHuman Body Structure from Cells to TissuesBlessy Amor UrmenetaÎncă nu există evaluări
- An Introduction To The Human BodyDocument38 paginiAn Introduction To The Human Bodyjonas hingcoÎncă nu există evaluări
- RH IncompatibilityDocument38 paginiRH IncompatibilitynamitaÎncă nu există evaluări
- What Is Dynamic Neuromuscular Stabilization (DNS) ?: How Is The Core Stabilized?Document5 paginiWhat Is Dynamic Neuromuscular Stabilization (DNS) ?: How Is The Core Stabilized?HONGJYÎncă nu există evaluări
- Cognitive Psychology Connecting Mind Research and Everyday Experience 4th Edition Goldstein Test BankDocument36 paginiCognitive Psychology Connecting Mind Research and Everyday Experience 4th Edition Goldstein Test Bankscrawlrootcapn0srm8100% (26)
- ColostomyDocument45 paginiColostomydrqiekiÎncă nu există evaluări
- Cardiovascular System Physiology LectureDocument28 paginiCardiovascular System Physiology LecturevincenzoÎncă nu există evaluări
- Introduction To Basic Pathology - 09.08.2023.ppt-1Document31 paginiIntroduction To Basic Pathology - 09.08.2023.ppt-1Abdur RaquibÎncă nu există evaluări
- BlastulaDocument4 paginiBlastulaCyanDesÎncă nu există evaluări
- Atlas Of: Human Body Ultrasound ScanningDocument575 paginiAtlas Of: Human Body Ultrasound ScanningGARY WILLIAMS CORTEZ PEREZÎncă nu există evaluări
- 20 - Pediatric Urinary DisordersDocument62 pagini20 - Pediatric Urinary DisordersKhaalid AbdirahmanÎncă nu există evaluări
- Causes and Diagnosis of SteatorrheaDocument43 paginiCauses and Diagnosis of SteatorrheaJohnRobynDiezÎncă nu există evaluări
- Human Health and Diseases PDFDocument61 paginiHuman Health and Diseases PDFnehaÎncă nu există evaluări
- Report Text Materi Dan SoalDocument7 paginiReport Text Materi Dan SoalShadrina ChaerunissaÎncă nu există evaluări
- Cell To BiosphereDocument38 paginiCell To BiospherezaiÎncă nu există evaluări
- Solutions - AIATS Medical-2016 Test-08 - (Code-A & B)Document19 paginiSolutions - AIATS Medical-2016 Test-08 - (Code-A & B)gnkstarÎncă nu există evaluări
- Module 3 The Cell Cycle PDFDocument8 paginiModule 3 The Cell Cycle PDFGlydelle Cabaldo100% (1)
- Animal and Plant CellsDocument40 paginiAnimal and Plant Cellsnika zanaÎncă nu există evaluări
- A Histopathological Study of Liver in 118 Cases of Cirrhosis 2167 0889 1000193 PDFDocument7 paginiA Histopathological Study of Liver in 118 Cases of Cirrhosis 2167 0889 1000193 PDFHemin HassanÎncă nu există evaluări
- Textbook Catalogue 2009Document52 paginiTextbook Catalogue 2009Lippincott Williams and Wilkins- Europe100% (2)
- Tutorial 3 - Lymphatic System PDFDocument4 paginiTutorial 3 - Lymphatic System PDFpizzaÎncă nu există evaluări
- Abdominal Wall DefectsDocument20 paginiAbdominal Wall DefectsxylomiteÎncă nu există evaluări
- Lectures No 4 Introduction & Method of Tissue Preparation & Specimen Reception & FixationDocument27 paginiLectures No 4 Introduction & Method of Tissue Preparation & Specimen Reception & FixationAbdallah AlasalÎncă nu există evaluări
- 4 Hodges and Tucker. Moving Differently in Pain. 2011Document9 pagini4 Hodges and Tucker. Moving Differently in Pain. 2011ningaxshopÎncă nu există evaluări
- Benign Prostatic Hyperplasia: A Case Analysis OnDocument70 paginiBenign Prostatic Hyperplasia: A Case Analysis OnAngelica RelanaÎncă nu există evaluări
- Cell (XI Grade)Document27 paginiCell (XI Grade)Ahmad LuthfyÎncă nu există evaluări
- CRANIAL BASE DEVELOPMENT STUDYDocument28 paginiCRANIAL BASE DEVELOPMENT STUDYPauly JinezÎncă nu există evaluări
- Hirschsprung PathophysiologyDocument4 paginiHirschsprung PathophysiologyJona SuarezÎncă nu există evaluări