Documente Academic
Documente Profesional
Documente Cultură
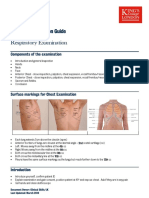
Procedure for THORACENTESIS: Patient Positioning and Local Anesthesia
Încărcat de
Ellie Marie Manlangit AguilarDescriere originală:
Titlu original
Drepturi de autor
Formate disponibile
Partajați acest document
Partajați sau inserați document
Vi se pare util acest document?
Este necorespunzător acest conținut?
Raportați acest documentDrepturi de autor:
Formate disponibile
Procedure for THORACENTESIS: Patient Positioning and Local Anesthesia
Încărcat de
Ellie Marie Manlangit AguilarDrepturi de autor:
Formate disponibile
Procedure for THORACENTESIS: Position of Patient: High Fowlers with legs hanging at the side of the bed.
The patient is to lean forward and to rest the arms on a table adjusted to the height of the the patients elbow Rationale: This position moves the scapulae anterolaterally, exposing most of the patients back. If sitting position cant be done, a lateral approach is selected: patient is propped up with a rolled towel placed lengthwise beneath the back with upper arms resting over the ear. Rationale: This position opens up the intercostal spaces. Alternative positions and areas are chosen when pleural effusion is loculated to provide for successful evacuated of loculated fluid. 1. After review of the old and new chest radiographs, thoracentesis can be perfomed. The fluid level is first percussed and the ribs in the region are palpated to identify the intercostal space through which the needle will be inserted. - The most appropriate site is the 7th intercostal space. (The site is localized by palpating the tip of the scapula with the patient sitting upright.) 2. Patient is prepped and draped. 3. Local anesthetic (e.g 1% lidocaine) is used to raise a wheal in the epidermis. - The most important point of view of the patient is that the procedure should be painless. 4. Pain is avoided by further advancing the needle and anesthetizing the periosteum over the 8 th rib, as well as the parietal pleura in the 7th intercostal space. - This is done by infiltrating the subcutaneous tissues and then guiding the needle over the superior margin of the 8th rib, remaining perpendicular to the rib. *DAMAGE TO THE INTERCOSTAL NEUROVASCULAR BUNDLE can be PREVENTED by maintaining a PERPENDICULAR ORIENTATION. The intercostals neurovascular bundle is located in the inercostal groove of the 7th rib. 5. At the level of the rib, infiltration of the tissue is alternated with aspiration with the syringe to ascertain when the pleural space has been reached. 6. Once fluid has been aspirated confirming that the needle has reached the pleural space, the needle is slowly withdrawn while a further 2 to 3 ml of local anesthesia is injected. - if procedure is done correctly, the parietal pleura will be well anesthetized. * IF FLUID CANNOT BE ASPIRATED, the attempt should be made to ANESTHETIZE AND ASPIRATE ONE INTERCOSTAL SPACE LOWER. THE RECOMMENDATION HOWEVER IS TO GO NO LOWER THAN THE 8TH INTERCOSTAL SPACE due to the risk of lacerating the LIVER (right) or the SPLEEN (left)-> lies adjacent to the bed of ribs 9 to 11.
7. Thoracentesis catheter inserted into the pleural space. - the catheter should be kept perpendicular to the chest wall to avoid inaverdent injury to the intercostals neurovascular bundle of the 8th rib. 8. Fluid is removed into a 60ml syringe and injected into a sterile bulb or bottle connected to the catheter with a stop-cock. 9. A CHEST RADIOGRAPH should be obtained subsequent to any attempt at thoracentesis. - to check for the presence of either a pneumothorax or residual fluid collection.
S-ar putea să vă placă și
- Geriatric Soap NoteDocument6 paginiGeriatric Soap Noteapi-282282363100% (6)
- Trusted Medical Answers-In Seconds.: Lipid DisordersDocument13 paginiTrusted Medical Answers-In Seconds.: Lipid DisordersMohammed shamiul Shahid100% (1)
- Basic Abdominal ExaminationDocument3 paginiBasic Abdominal Examinationcpradheep100% (1)
- Special Health Reports - Harvard HealthDocument9 paginiSpecial Health Reports - Harvard HealthBassuÎncă nu există evaluări
- Abdominal Examination ProcedureDocument5 paginiAbdominal Examination ProcedureAnamul hossainÎncă nu există evaluări
- Respiratory Examination GuideDocument4 paginiRespiratory Examination Guiderhea100% (2)
- ThoracentesisDocument25 paginiThoracentesisroger100% (2)
- Respiratory Examination: The Position of The PatientDocument24 paginiRespiratory Examination: The Position of The PatientMuhammed Barznji100% (1)
- Abdominal Exam GuideDocument5 paginiAbdominal Exam GuideNesma AdelÎncă nu există evaluări
- Fundamental of Nursing QuizDocument15 paginiFundamental of Nursing QuizDr. Jayesh Patidar100% (1)
- ElbowDocument7 paginiElbowapi-302398226Încă nu există evaluări
- Abdominal Exam Guide: Palpation, Inspection & Surface MarkingsDocument4 paginiAbdominal Exam Guide: Palpation, Inspection & Surface MarkingsPhysician AssociateÎncă nu există evaluări
- LymphaticDocument52 paginiLymphaticlemuel_queÎncă nu există evaluări
- Infection of The Skin, Soft Tissue, Etc.Document84 paginiInfection of The Skin, Soft Tissue, Etc.fmds100% (1)
- Head To Toe Physical AssessmentDocument9 paginiHead To Toe Physical Assessmentthe studentÎncă nu există evaluări
- Oral Surgery and InfectionsDocument32 paginiOral Surgery and InfectionsTheSuperJayR100% (1)
- Bed PositionsDocument4 paginiBed PositionsJessa Kris RialubinÎncă nu există evaluări
- Lumber Puncture ProcedureDocument8 paginiLumber Puncture ProcedureDimpal ChoudharyÎncă nu există evaluări
- Enteral Nutrition Administration Inconsistent With Needs (NI-2.6)Document2 paginiEnteral Nutrition Administration Inconsistent With Needs (NI-2.6)Hasna KhairunnisaGIZIÎncă nu există evaluări
- Bullets CDDocument2 paginiBullets CDJonas Marvin AnaqueÎncă nu există evaluări
- NCP For Dengue Hemorrhagic FeverDocument14 paginiNCP For Dengue Hemorrhagic FeverKim Celeste Matulac100% (3)
- Lumber Puncture ProcedureDocument8 paginiLumber Puncture ProcedureDimpal ChoudharyÎncă nu există evaluări
- Pre EclampsiaDocument17 paginiPre Eclampsiachristeenangela0% (1)
- Thorax Exam Surface MarkingsDocument4 paginiThorax Exam Surface Markingsdidutza91Încă nu există evaluări
- Lumbar Puncture and Bone Marrow Aspiration ProceduresDocument25 paginiLumbar Puncture and Bone Marrow Aspiration Proceduresomar kmr97Încă nu există evaluări
- No. 3 Lumbar PunctureDocument4 paginiNo. 3 Lumbar PunctureGrant Wynn ArnucoÎncă nu există evaluări
- Spinal AnaesthesiaDocument9 paginiSpinal Anaesthesiaapi-142637023Încă nu există evaluări
- Osce: Outlet Forceps ExtractionDocument2 paginiOsce: Outlet Forceps ExtractionValerie Gonzaga-CarandangÎncă nu există evaluări
- Tension PneumothoraxDocument3 paginiTension PneumothoraxariefÎncă nu există evaluări
- 2-Checklist For Pelvis AssessmentDocument3 pagini2-Checklist For Pelvis AssessmentGazala ParveenÎncă nu există evaluări
- Abdomen exam guide under 40 charsDocument5 paginiAbdomen exam guide under 40 charsdidutza91Încă nu există evaluări
- Rigid Esophagoscopy (Complete)Document4 paginiRigid Esophagoscopy (Complete)Yukiko CalimutanÎncă nu există evaluări
- Name: Werly Eka Saputri (21115060) Kartika Apriliyani (21115052)Document4 paginiName: Werly Eka Saputri (21115060) Kartika Apriliyani (21115052)Werly Eka LiaÎncă nu există evaluări
- Macloaed Only ExaminationDocument3 paginiMacloaed Only ExaminationTahir AliÎncă nu există evaluări
- Anal FistulasDocument9 paginiAnal FistulasikeernawatiÎncă nu există evaluări
- Arthrotomy of KneeDocument9 paginiArthrotomy of KneecmonmanÎncă nu există evaluări
- Clinical Examination of Respiratory SystemDocument12 paginiClinical Examination of Respiratory SystemAmit PandyaÎncă nu există evaluări
- Chest Tube InsertionDocument4 paginiChest Tube InsertionHugo ARÎncă nu există evaluări
- Abdominal Exam StepsDocument4 paginiAbdominal Exam StepsRonaldoÎncă nu există evaluări
- Inferior Alveolar TechniqueDocument8 paginiInferior Alveolar Techniquebalab2311Încă nu există evaluări
- Procedure Checklist Chapter 35: Performing Percussion, Vibration, and Postural DrainageDocument2 paginiProcedure Checklist Chapter 35: Performing Percussion, Vibration, and Postural DrainagejthsÎncă nu există evaluări
- LP Procedure StepsDocument3 paginiLP Procedure StepsChristian Anthony L. GamoloÎncă nu există evaluări
- Hernia ExaminationDocument3 paginiHernia Examinationjackfruit5887Încă nu există evaluări
- Episiotomy: Surgical Cut During ChildbirthDocument4 paginiEpisiotomy: Surgical Cut During Childbirthnursing school0% (1)
- Trauma, Shock, Head Injuries and Burns 51Document1 paginăTrauma, Shock, Head Injuries and Burns 51refree2wc3303Încă nu există evaluări
- Complete Respiratory Examination Checklist 365Document5 paginiComplete Respiratory Examination Checklist 365mohammed alrubaiaanÎncă nu există evaluări
- Cme Trauma Management ZakwanDocument44 paginiCme Trauma Management ZakwansyasyaÎncă nu există evaluări
- Css - Radio Jeliya FixDocument16 paginiCss - Radio Jeliya FixJelya SafitriÎncă nu există evaluări
- Dr.K.sellahewa Cardiovascular System ExaminationDocument8 paginiDr.K.sellahewa Cardiovascular System ExaminationNilaaharan RobinsonÎncă nu există evaluări
- Cervical Internal Examination ExplanationDocument5 paginiCervical Internal Examination ExplanationKing Aldus ConstantinoÎncă nu există evaluări
- What Are The Physical Examination On Monitoring The Labour?Document2 paginiWhat Are The Physical Examination On Monitoring The Labour?Nurfi Resni Fitra RamdaÎncă nu există evaluări
- Harvesting Vascularized Fibula Flap & Deep Inferior Epigastric Perforators (Diep)Document31 paginiHarvesting Vascularized Fibula Flap & Deep Inferior Epigastric Perforators (Diep)Putri PurwanthiÎncă nu există evaluări
- Thomas Jonnesco - Remarks On General Spinal Analgesia (1909) .Document6 paginiThomas Jonnesco - Remarks On General Spinal Analgesia (1909) .BigBoss_GRUÎncă nu există evaluări
- Epidural AnesthesiaDocument6 paginiEpidural AnesthesiaBibek SutradharÎncă nu există evaluări
- Chest Tube Placement (Adult)Document8 paginiChest Tube Placement (Adult)Ariane Joyce SalibioÎncă nu există evaluări
- Stagiaire's Guide To General Surgery OSCEsDocument36 paginiStagiaire's Guide To General Surgery OSCEsMawÎncă nu există evaluări
- The female pelvis, fetal skull diameters and clinical pelvimetryDocument9 paginiThe female pelvis, fetal skull diameters and clinical pelvimetryMohammed AbdÎncă nu există evaluări
- Abdomen MCQDocument24 paginiAbdomen MCQTatyanna Rammouz100% (1)
- Proning Patients Checklist: Staff Requirements - MinimumDocument3 paginiProning Patients Checklist: Staff Requirements - MinimumAdam KurniaÎncă nu există evaluări
- PE CompreDocument5 paginiPE Comprejustme12345mÎncă nu există evaluări
- "Krishna Institute of Medical Sciences ": Deemed University, Karad."Document12 pagini"Krishna Institute of Medical Sciences ": Deemed University, Karad."Savita HanamsagarÎncă nu există evaluări
- Thoracocentasis: INTRODUCTION:-Thoracentasis Also Known As The Thoracocentasis or Plural Tap Is AnDocument7 paginiThoracocentasis: INTRODUCTION:-Thoracentasis Also Known As The Thoracocentasis or Plural Tap Is AnaparnaÎncă nu există evaluări
- RespDocument10 paginiRespvonon35132Încă nu există evaluări
- Lumbar Puncture ReportDocument5 paginiLumbar Puncture ReportTweenie DalumpinesÎncă nu există evaluări
- Insertion Nasogastric Tube: Catheterizing The Female & Male Urinary Bladder (Straight & Indwelling)Document4 paginiInsertion Nasogastric Tube: Catheterizing The Female & Male Urinary Bladder (Straight & Indwelling)ad-adÎncă nu există evaluări
- Version 2.0 04/08/2020Document12 paginiVersion 2.0 04/08/2020ArlanosaurusÎncă nu există evaluări
- A Manual of the Operations of Surgery: For the Use of Senior Students, House Surgeons, and Junior PractitionersDe la EverandA Manual of the Operations of Surgery: For the Use of Senior Students, House Surgeons, and Junior PractitionersÎncă nu există evaluări
- Echinacea SPP MonographDocument2 paginiEchinacea SPP MonographOliver Rathbone100% (1)
- CHROMagar Candida Plus IFUDocument13 paginiCHROMagar Candida Plus IFUIsa LópezÎncă nu există evaluări
- ADC Part 1 - TG Keynotes II v1.0 PDFDocument17 paginiADC Part 1 - TG Keynotes II v1.0 PDFDrSaif Ullah KhanÎncă nu există evaluări
- Government and Private Hospitals in BhopalDocument3 paginiGovernment and Private Hospitals in BhopalDeepak Kumar RajakÎncă nu există evaluări
- Central Venous Pressure (CVP) Monitoring Using A Water ManometerDocument5 paginiCentral Venous Pressure (CVP) Monitoring Using A Water ManometerBsBs A7medÎncă nu există evaluări
- Renal Replacement TherapyDocument23 paginiRenal Replacement TherapybgfhnfgÎncă nu există evaluări
- HeartSave AED Brochure - SemiDocument14 paginiHeartSave AED Brochure - SemiJuan Sebastián Sánchez LópezÎncă nu există evaluări
- Eucalyptus OilDocument17 paginiEucalyptus OilSorinGeorgeÎncă nu există evaluări
- Stem Cell Therapy and EthicsDocument2 paginiStem Cell Therapy and EthicsRaniya Khan [Student]Încă nu există evaluări
- Review Article: Caffeic Acid Phenethyl Ester and Therapeutic PotentialsDocument10 paginiReview Article: Caffeic Acid Phenethyl Ester and Therapeutic PotentialsDwi wahyuniÎncă nu există evaluări
- Shashwat Ayu 2024 - DR Manish SinghDocument15 paginiShashwat Ayu 2024 - DR Manish Singhmanish singhÎncă nu există evaluări
- Test Bank For Database Concepts 6th Edition KroenkeDocument24 paginiTest Bank For Database Concepts 6th Edition KroenkeJasonFitzpatrickozyb100% (38)
- 2022 SCO OneCare PM Prior Auth Table 3.1.2022-1Document15 pagini2022 SCO OneCare PM Prior Auth Table 3.1.2022-1joshnemoÎncă nu există evaluări
- Diastema Closure PDFDocument5 paginiDiastema Closure PDFsimon yonathanÎncă nu există evaluări
- Aloe Vera (Gel) Other Aloe SPP.: Aloe Vera (L.) Burm.f., A. Arborescens Mill. andDocument3 paginiAloe Vera (Gel) Other Aloe SPP.: Aloe Vera (L.) Burm.f., A. Arborescens Mill. andRiani EkawatiÎncă nu există evaluări
- Physical & Multiple Disability ChecklistDocument3 paginiPhysical & Multiple Disability ChecklistGheylhu AmorÎncă nu există evaluări
- Breast Augmentation and Breast ReductionDocument13 paginiBreast Augmentation and Breast ReductionDjlatino LatinoÎncă nu există evaluări
- Immediate Life Support - NewDocument67 paginiImmediate Life Support - NewTalhaÎncă nu există evaluări
- Beyond Bowels: Understanding Co-existing Symptoms in IBSDocument8 paginiBeyond Bowels: Understanding Co-existing Symptoms in IBSparthibanemails5779Încă nu există evaluări
- Lec 9 Antihuman Globulin TestingDocument9 paginiLec 9 Antihuman Globulin TestingMelaine Grace Gemoranion GeopanoÎncă nu există evaluări