Documente Academic
Documente Profesional
Documente Cultură
Functions and Properties of Blood - Plasma - Blood Cell Production - Erythrocytes - Blood Types - Leukocytes - Hemostasis (Stoppage of Bleeding)
Încărcat de
vanderphys0 evaluări0% au considerat acest document util (0 voturi)
105 vizualizări47 paginiThis document provides a summary of the key topics covered in Chapter 18 on the circulatory system and blood. It discusses the functions and properties of blood, the components of blood including plasma, red blood cells, white blood cells, and platelets. It covers the production of blood cells through hematopoiesis, the different blood types, and some common blood disorders like sickle cell anemia, thalassemia, polycythemia, and anemia.
Descriere originală:
MCAT prep
Titlu original
18 Blood
Drepturi de autor
© © All Rights Reserved
Formate disponibile
PPT, PDF, TXT sau citiți online pe Scribd
Partajați acest document
Partajați sau inserați document
Vi se pare util acest document?
Este necorespunzător acest conținut?
Raportați acest documentThis document provides a summary of the key topics covered in Chapter 18 on the circulatory system and blood. It discusses the functions and properties of blood, the components of blood including plasma, red blood cells, white blood cells, and platelets. It covers the production of blood cells through hematopoiesis, the different blood types, and some common blood disorders like sickle cell anemia, thalassemia, polycythemia, and anemia.
Drepturi de autor:
© All Rights Reserved
Formate disponibile
Descărcați ca PPT, PDF, TXT sau citiți online pe Scribd
0 evaluări0% au considerat acest document util (0 voturi)
105 vizualizări47 paginiFunctions and Properties of Blood - Plasma - Blood Cell Production - Erythrocytes - Blood Types - Leukocytes - Hemostasis (Stoppage of Bleeding)
Încărcat de
vanderphysThis document provides a summary of the key topics covered in Chapter 18 on the circulatory system and blood. It discusses the functions and properties of blood, the components of blood including plasma, red blood cells, white blood cells, and platelets. It covers the production of blood cells through hematopoiesis, the different blood types, and some common blood disorders like sickle cell anemia, thalassemia, polycythemia, and anemia.
Drepturi de autor:
© All Rights Reserved
Formate disponibile
Descărcați ca PPT, PDF, TXT sau citiți online pe Scribd
Sunteți pe pagina 1din 47
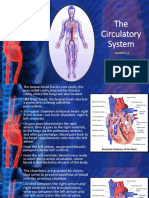
Chapter 18
The Circulatory System: Blood
Functions and properties of
blood
Plasma
Blood cell production
Erythrocytes
Blood types
Leukocytes
Hemostasis (stoppage of
bleeding)
Functions and Properties of Blood
Functions in respiration, nutrition, waste
elimination, thermoregulation, immune defense,
water and pH balance, etc.
Adults have 4-6 L of blood
plasma, a clear extracellular fluid
formed elements (blood cells and platelets)
Properties of blood
viscosity (resistance to flow)
osmolarity (total molarity of dissolved particles)
if incorrect causes high BP or edema & low BP
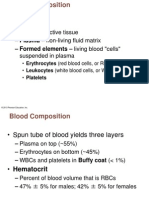
Formed Elements of Blood
Hematocrit
Centrifuging blood forces formed elements to separate
from plasma
Hematocrit is % of total volume that is cells
Plasma and Plasma Proteins
Plasma is a mixture of proteins, enzymes, nutrients,
wastes, hormones, and gases
if allowed to clot, what remains is called serum
All plasma proteins formed by liver except globulins
(produced by plasma cells)
Albumins are most abundant plasma protein
contributes to viscosity and osmolarity and influences blood
pressure, flow and fluid balance
Fibrinogen is precursor of fibrin threads that help form
blood clots
Globulins provide immune system defenses
Nonprotein Components of Plasma
Plasma contains nitrogenous compounds
amino acids from dietary protein or tissue breakdown
nitrogenous wastes (urea) are toxic end products of
catabolism
normally removed from the blood by the kidneys
Nutrients (glucose, vitamins, fats, minerals, etc)
Some O
2
and CO
2
are transported in plasma
Many electrolytes are found in plasma
Na
+
makes up 90% of plasma cations accounting
for more of bloods osmolarity than any other
solute
Blood Cell Production (Hematopoiesis)
Hemopoietic tissues produce blood cells
yolk sac in vertebrate embryo produce stem cells that colonize
fetal bone marrow, liver, spleen & thymus
liver stops producing blood cells at birth, but spleen and thymus
remain involved with WBC production
lymphoid hemopoiesis occurs in widely distributed lymphoid
tissues (thymus, tonsils, lymph nodes, spleen & peyers patches in
intestines)
red bone marrow produces RBCs, WBCs and platelets
stem cells called hemocytoblasts multiply continually & are pluripotent
(capable of differentiating into multiple cell lines)
committed cells are destined to continue down one specific cell line
Stimulated by erythropoietin, thrombopoietin & colony-
stimulating factors (CSFs)
Hemopoiesis
Granulocytes
Erythrocyte Production
Erythropoiesis produces 2.5 million RBCs/second
First committed cell is proerythroblast
has receptors for erythropoietin (EPO) from kidneys
Erythroblasts multiply & synthesize hemoglobin
Nucleus degenerates to form a reticulocyte
named for fine network of endoplasmic reticulum
enters bloodstream as 0.5 to 1.5% of circulating RBCs
Development takes 3-5 days & involves
reduction in cell size, increase in cell number, synthesis of
hemoglobin & loss of nucleus
Erythrocyte Homeostasis
Classic negative feedback
control
drop in RBC count causes
hypoxemia to kidneys
erythropoietin production
stimulation of bone marrow
RBC count in 3-4 days
Stimulus for erythropoiesis
low levels of atmospheric O
2
increase in exercise
hemorrhaging
Nutritional Needs for Erythropoiesis
Iron is key nutritional requirement for erythropoiesis
lost daily through urine, feces, and bleeding
men 0.9 mg/day and women 1.7 mg/day
low absorption rate requires consumption of 5-20 mg/day
dietary iron in 2 forms: ferric (Fe
3+
) & ferrous (Fe
2+
)
stomach acid converts Fe+3 to absorbable Fe+2
gastroferritin from stomach binds Fe+2 & transports it to intestine
absorbed into blood & binds to transferrin to travel
bone marrow uses to make hemoglobin, muscle used to make
myoglobin and all cells use to make cytochromes in mitochondria
liver binds surplus to apoferritin to create ferritin for storage
B12 & folic acid (for rapid cell division) and vitamin C
& Cu for cofactors for enzymes synthesizing RBCs
Iron Absorption, Transport & Storage
Leukocyte Production (Leukopoiesis)
Committed cell types -- B & T progenitors and
granulocyte-macrophage colony-forming units
possess receptors for colony-stimulating factors
released by mature WBCs in response to infections
RBC stores & releases granulocytes & monocytes
Some lymphocytes leave bone marrow unfinished
go to thymus to complete their development (T cells)
Circulating WBCs do not stay in bloodstream
granulocytes leave in 8 hours & live 5 days longer
monocytes leave in 20 hours, transform into macrophages and
live for several years
WBCs providing long-term immunity last decades
Platelet Production (Thrombopoiesis)
Hemocytoblast that develops receptors for
thrombopoietin from liver or kidney becomes
megakaryoblast
Megakaryoblast repeatedly replicates its DNA
without dividing
forms gigantic cell called megakaryocyte (100 m in
diameter that remains in bone marrow)
Infoldings of megakaryocyte cytoplasm splits off
cell fragments that enter the bloodstream as
platelets (live for 4 days)
some stored in spleen & released as needed
Megakaryocytes & Platelets
Erythrocytes (RBCs)
Disc-shaped cell with thick rim
7.5 M diameter & 2.0 m thick at rim
Major function is gas transport
lost all organelles during maturation so
has increased surface area/volume ratio
increases diffusion rate of substances in & out of cell
33% of cytoplasm is hemoglobin (Hb)
O
2
delivery to tissue and CO
2
transport back to lungs
contains enzyme, carbonic anhydrase (CAH)
produces carbonic acid from CO2 and water
important role in gas transport & pH balance
Erythrocytes on a Needle
Hemoglobin Structure
Hemoglobin consists of 4
protein chains called
globins (2 alpha & 2 beta)
Each protein chain is
conjugated with a heme
group which binds oxygen
to ferrous ion (Fe+2)
Hemoglobin molecule can
carry four O2
Fetal hemoglobin
gamma instead of beta chains
Erythrocytes and Hemoglobin
RBC count & hemoglobin concentration indicate
the amount of oxygen the blood can carry
hematocrit is % of blood volume consisting of cells
men 42-52% cells; women 37-48% cells
hemoglobin concentration of whole blood
men 13-18g/dL; women 12-16g/dL
RBC count
men 4.6-6.2 million/L; women 4-2-5.4 million/L
Values are lower in women
androgens stimulate RBC production
women have periodic menstrual losses
Erythrocyte Death & Disposal
RBCs live for 120 days
membrane fragility -- lysis in
narrow channels in the spleen
Macrophages in spleen
digest membrane bits
separate heme from globin
hydrolyze globin (amino acids)
remove iron from heme
convert heme to biliverdin
convert biliverdin to bilirubin
becomes bile product in feces
Erythrocyte Disorders
Polycythemia is an excess of RBC
primary polycythemia is due to cancer of
erythropoietic cell line in the red bone marrow
RBC count as high as 11 million/L; hematocrit of 80%
secondary polycythemia from dehydration,
emphysema, high altitude, or physical conditioning
RBC count only up to 8 million/L
Dangers of polycythemia
increased blood volume, pressure and viscosity can
lead to embolism, stroke or heart failure
Anemia - Deficiency of RBCs or Hb
Causes of anemia
inadequate erythropoiesis or hemoglobin synthesis
inadequate vitamin B12 (cobalamin) or folate (B9, a derivative of B12)
from poor nutrition
lack of intrinsic factor due to autoimmune destruction of parietal cells
(pernicious anemia)
iron-deficiency anemia
kidney failure & insufficient erythropoietin hormone
aplastic anemia is complete cessation (cause unknown)
hemorrhagic anemias from loss of blood
hemolytic anemias from RBC destruction
Effects of anemia
tissue hypoxia and necrosis (short of breath & lethargic)
low blood osmolarity (tissue edema)
low blood viscosity (heart races & pressure drops)
Sickle-Cell Disease & Thalassemia
Sickle-Cell is hereditary Hb defect of African Americans
autosomal recessive allele modifies hemoglobin structure
homozygous recessive for HbS have sickle-cell disease
heterozygous recessive for HbS have sickle-cell trait
sickle-cell disease individual has shortened life
HbS turns to gel in low oxygen concentrations, agglutinating cells and
blocking vessels
intense pain, heart failure, paralysis, anemia, hypoxemia
HbS is indigestible to malaria parasites so gene persists despite
its harmful effects to the homozygous individuals
Thalassemia is hereditary Hb defect seen among people
of Mediterranean area
autosomal recessive
deficiency or absence of alpha or beta hemoglobin
RBC counts less than 2 million cells/L
Blood Types
RBC antigens
called agglutinogens A & B
inherited combinations of
proteins, glycoproteins and
glycolipids on red blood cell
Plasma antibodies
called agglutinins anti-A & -B
gamma globulins in blood
plasma that recognize (stick to)
foreign agglutinogens on RBCs
responsible for RBC agglutination in mismatched
blood transfusions
The ABO Group
ABO blood type is determined by presence or absence
of agglutinogens A & B on RBCs
blood type A person has A agglutinogens, blood type B person has
B agglutinogens, AB has both & blood type O has neither
blood type O is the most common; AB the rarest
Agglutinins appear in the plasma 2-8 months after birth &
at maximum concentration at 10 yr.
agglutinins A and/or B, both or none are in plasma
you do not have those that would react against your own
agglutinogens
each agglutinin, usually IgM, can attach to several agglutinogens
at the same time causing agglutination (clumping)
Agglutination of Erythrocytes
Transfusions
Donor
Reciepient
O A B AB
O x
A x x
B x x
AB x x x x
Mismatched Transfusion Reaction
Agglutinated RBCs
block blood vessels
& rupture
free Hb can block kidney
tubules & cause death
Concept of universal
donors and recipients is obsolete
AB was called universal recipient since it lacks both
antibody A and B; O was called universal donor
problem was donors plasma could have antibodies
solution is giving packed cells with minimum plasma
The Rh Group
Rh or D agglutinogens discovered in rhesus monkey in 1940
blood type is Rh+ if agglutinogens present on RBCs
Rh frequencies vary among ethnic groups
Anti-D agglutinins are not normally present in blood
form only in individuals exposed to Rh+ blood
Rh- pregnant woman carrying an Rh+ fetus or blood transfusion of Rh+
blood
no problems result with either the first transfusion or the first pregnancy
2
nd
time: abortion or miscarriage
hemolytic disease of the newborn (erythroblastosis fetalis) occurs if mother has
formed antibodies & is pregnant with 2nd Rh+ child
RhoGAM is given to pregnant woman to prevent antibody
formation and prevent any future problems
RhoGAM binds fetal agglutinogens in her blood so she will not form
antibodies against them during the pregnancy
Hemolytic Disease of Newborn
Mothers antibodies attack fetal blood causing severe anemia
& toxic brain syndrome from excessive bilirubin in blood
treatment is phototherapy to degrade bilirubin or exchange
transfusion to completely replace infants blood
Leukocyte Descriptions (WBCs)
Granulocytes
eosinophils - pink-orange granules & bilobed nucleus (2-4%)
basophils - abundant, dark violet granules (<1%)
large U- to S-shaped nucleus hidden by granules
neutrophils - multilobed nucleus (60-70%)
fine reddish to violet granules in cytoplasm
Agranulocytes
lymphocytes - round, uniform dark violet nucleus (25-33%)
variable amounts of bluish cytoplasm (scanty to abundant)
monocytes - kidney- or horseshoe-shaped nucleus (3-8%)
large cell with abundant cytoplasm
Granulocyte Functions
Neutrophils
in bacterial infections
most abundant leukocyte
phagocytosis of bacteria
releases antimicrobial chemicals
Eosinophils
in parasitic infections or allergies
phagocytosis of antigen-antibody complexes, allergens &
inflammatory chemicals
release enzymes destroy parasites such as worms
Basophils
in allergic reactions (anaphylaxis) and inflammation
cooperate with mast cells
secrete histamine (vasodilator)
secrete heparin (anticoagulant)
Agranulocyte Functions
Lymphocytes
in diverse infections & immune responses
destroy cancer & foreign cells & virally infected cells
present antigens to activate other immune cells
coordinate actions of other immune cells
secrete antibodies & provide immune memory
Monocytes
in viral infections & inflammation
differentiate into macrophages
phagocytize pathogens and debris
present antigens to activate other immune cells
Abnormalities of Leukocyte Count
Leukopenia = low WBC count (<5000/L)
causes -- radiation, poisons, infectious disease
effects -- elevated risk of infection
Leukocytosis = high WBC count (>10,000/L)
causes -- infection, allergy & disease
differential count -- distinguishes % of each cell type
Leukemia = cancer of hemopoietic tissue
myeloid and lymphoid -- uncontrolled WBC production
acute and chronic -- death in either months or 3 years
effects -- normal cell % disrupted, patient subject to
opportunistic infection, anemia & impaired clotting
Hemostasis - The Control of Bleeding
Effective at closing breaks in small vessels
3 hemostatic mechanisms all involve platelets
Platelets
Small fragments of megakaryocyte cytoplasm
2-4 m diameter & containing granules
pseudopods provide amoeboid movement & phagocytosis
Normal Count -- 130,000 to 400,000 platelets/L
Functions
secrete clotting factors, growth factors for endothelial
repair, and vasoconstrictors in broken vessels
form temporary platelet plugs
dissolve old blood clots
phagocytize bacteria
attract WBCs to sites of inflammation
Vascular Spasm
Prompt constriction of a broken vessel
Triggers for a vascular spasm
some pain receptors directly innervate constrictors
lasts only a few minutes
injury to smooth muscle
longer-lasting constriction
platelets release serotonin, chemical vasoconstrictor
Provides time for other 2 mechanisms to work
Platelet Plug Formation
Normal endothelium very smooth & coated with
prostacyclin (platelet repellent)
Broken vessel exposes rough surfaces of collagen
Platelet plug formation begins
platelet pseudopods stick to damaged vessel and other platelets --
pseudopods contract and draw walls of vessel together forming a
platelet plug
platelets degranulate releasing a variety of substances
serotonin is a vasoconstrictor
adenosine diphosphate (ADP) attracts & degranulates more platelets
thromboxane A2, an eicosanoid that promotes aggregation,
degranulation & vasoconstriction
Positive feedback cycle is active until break in vessel is
sealed
Coagulation
Clotting is the most effective defense against bleeding ---
needs to be quick but accurate
conversion of plasma protein fibrinogen into insoluble
fibrin threads which form framework of clot
Procoagulants or clotting factors (inactive form produced
by the liver) are present in the plasma
activate one factor and it will activate the next to form a
reaction cascade
Factors released by the tissues cause the extrinsic
cascade pathway to begin (damaged vessels)
Factors found only in the blood itself cause the intrinsic
cascade pathway to begin (platelet degranulation)
Both cascades normally occur together
Coagulation Pathways
Extrinsic pathway
initiated by tissue
thromboplastin
cascade from factor
VII to V to X
Intrinsic pathway
initiated by factor XII
cascade from factor XI
to IX to VIII to X
Calcium is required
for either pathway
15 seconds 3-6 minutes
Enzyme Amplification in Clotting
Rapid clotting occurs since each activated enzyme
produces a large number of enzyme molecules in the
following step.
Completion of Coagulation
Coagulation is completed because of the formation
of enzymes in a stepwise fashion
Factor X produces prothrombin activator
Prothrombin activator
converts prothrombin
to thrombin
Thrombin converts
fibrinogen into fibrin
Positive feedback occurs as thrombin speeds up the
formation of prothrombin activator
The Fate of Blood Clots
Clot retraction occurs within 30 minutes
pseudopods of platelets contract condensing the clot
Platelet-derived growth factor is secreted by
platelets & endothelial cells
mitotic stimulant for fibroblasts and smooth muscle to
multiply & repair the damaged vessel
Fibrinolysis or dissolution of a clot
factor XII speeds up the formation of kallikrein enzyme
kallikrein converts plasminogen into plasmin, a
fibrin-dissolving enzyme or clot buster
Blood Clot Dissolution
Positive feedback occurs
Plasmin promotes formation of kallikrein
Positive
Feedback
Prevention of Inappropriate Coagulation
Platelet repulsion
platelets do not adhere to prostacyclin-coating
Thrombin dilution
normally diluted by rapidly flowing blood
heart slowing in shock can result in clot formation
Natural anticoagulants
antithrombin produced by the liver deactivates
thrombin before it can act on fibrinogen
heparin secreted by basophils & mast cells
interferes with formation of prothrombin activator
Coagulation Disorders
Thrombocytopenia
platelet count below 100,000/L (bruise easily)
Hemophilia
genetic lack of any clotting factor that affects
coagulation
X-linked recessive in males (inherit from mother)
hemophilia A is missing factor VIII (83% of cases)
hemophilia B is missing factor IX (15% of cases)
physical exertion causes bleeding & excruciating pain
transfusion of plasma or purified clotting factors
factor VIII now produced by transgenic bacteria
Coagulation Disorders
Unwanted coagulation
thrombosis = abnormal clotting in unbroken vessel
embolism = unwanted clot traveling in a vessel
Infarction or tissue death may occur if clot
blocks blood supply to an organ (MI or stroke)
650,000 Americans die annually of thromboembolism
Disseminated intravascular coagulation (DIC)
widespread clotting of blood within unbroken vessels
triggered by bacteria (septicemia) or if blood slows
down or stops as in cardiac arrest
S-ar putea să vă placă și
- Lecture 2-Blood RBC WBCDocument51 paginiLecture 2-Blood RBC WBCsamayaÎncă nu există evaluări
- The Circulatory System: BloodDocument59 paginiThe Circulatory System: BloodKristian Dave DivaÎncă nu există evaluări
- Anatomy and Physiology of BLOOD: Preet KaurDocument37 paginiAnatomy and Physiology of BLOOD: Preet KaurPreet KaurÎncă nu există evaluări
- BloodDocument80 paginiBloodHem Chandra ShahÎncă nu există evaluări
- BloodDocument76 paginiBloodKerby Dela Fuente Alison100% (1)
- CVS BloodDocument39 paginiCVS BloodMohan GuptaÎncă nu există evaluări
- BloodDocument49 paginiBloodDale TelgenhoffÎncă nu există evaluări
- Case 11Document63 paginiCase 11حكيم العجلانÎncă nu există evaluări
- The Circulatory System: BloodDocument69 paginiThe Circulatory System: BloodMozesCuateÎncă nu există evaluări
- BLOOD LecDocument46 paginiBLOOD LecGrape JuiceÎncă nu există evaluări
- AnaemiasDocument60 paginiAnaemiasbvkjtzrvnyÎncă nu există evaluări
- 1 BloodDocument77 pagini1 BloodVisaNathan100% (1)
- BLOOD Update-1Document56 paginiBLOOD Update-1ahmadfadi343Încă nu există evaluări
- Blood Cells, Immunity and Blood ClottingDocument65 paginiBlood Cells, Immunity and Blood Clottingmunaamuummee100% (1)
- Blood: Cardiovascular SystemDocument75 paginiBlood: Cardiovascular SystemTina MinottÎncă nu există evaluări
- Haemopoiesis: Composition of Whole Blood & Its ComponentsDocument8 paginiHaemopoiesis: Composition of Whole Blood & Its ComponentsSafiya JamesÎncă nu există evaluări
- Topics of This Lecture: RBC: - Structural Characteristics - Hemoglobin - Erythropoiesis - Erythrocytes DestructionDocument23 paginiTopics of This Lecture: RBC: - Structural Characteristics - Hemoglobin - Erythropoiesis - Erythrocytes DestructionHashim GhazoÎncă nu există evaluări
- Hematologic DisordersDocument30 paginiHematologic DisordersUday Kumar100% (1)
- PSG 712 Blood-1Document54 paginiPSG 712 Blood-1preciousÎncă nu există evaluări
- Hematology 2020Document63 paginiHematology 2020odiodi57Încă nu există evaluări
- Body Fluids and Their Circulation 1Document96 paginiBody Fluids and Their Circulation 1sanmathiÎncă nu există evaluări
- Blood: - Hematopoiesis (Hemopoiesis) : Blood CellDocument5 paginiBlood: - Hematopoiesis (Hemopoiesis) : Blood Cellflay1618Încă nu există evaluări
- Physiology of Blood: Ratna Kusumawati Department of Physiology, Faculty of Medicine Universitas Sebelas Maret SurakartaDocument60 paginiPhysiology of Blood: Ratna Kusumawati Department of Physiology, Faculty of Medicine Universitas Sebelas Maret SurakartaZidaneÎncă nu există evaluări
- Physiology of Blood: Ratna Kusumawati Department of Physiology, Faculty of Medicine Universitas Sebelas Maret SurakartaDocument65 paginiPhysiology of Blood: Ratna Kusumawati Department of Physiology, Faculty of Medicine Universitas Sebelas Maret SurakartaRizal AbdurrahmanÎncă nu există evaluări
- Functions of BloodDocument12 paginiFunctions of BloodAngieRamirezÎncă nu există evaluări
- Blood: - The Only Fluid Tissue in The Human Body - Classified As A Connective TissueDocument39 paginiBlood: - The Only Fluid Tissue in The Human Body - Classified As A Connective TissueJorÎncă nu există evaluări
- 1-Blood Composition and FunctionDocument43 pagini1-Blood Composition and FunctionKaleem Mohammad100% (2)
- Blood: - Enzymes, E.G. Certain Clotting FactorsDocument14 paginiBlood: - Enzymes, E.G. Certain Clotting FactorsDerrick kinyaÎncă nu există evaluări
- Introduction To HematologyDocument95 paginiIntroduction To HematologyAhmad Farhan Hassan0% (1)
- Chapter 4 Blood Coagulation and Coagulation DisordersDocument27 paginiChapter 4 Blood Coagulation and Coagulation DisordersdaisysintszwaiÎncă nu există evaluări
- Red Blood Cells, Anemia, and PolycythemiaDocument7 paginiRed Blood Cells, Anemia, and PolycythemiaShi no Me100% (1)
- LEC3Document26 paginiLEC3Jessica StewartÎncă nu există evaluări
- Blood: Group 1Document25 paginiBlood: Group 1Arian May MarcosÎncă nu există evaluări
- Biology Part-1 NotesDocument59 paginiBiology Part-1 NotesgjbxÎncă nu există evaluări
- Physio. D. Suroor. L1. BloodDocument24 paginiPhysio. D. Suroor. L1. Bloodزين العابدين محمد عويشÎncă nu există evaluări
- RBC DISORDERS Part I VR 2022Document63 paginiRBC DISORDERS Part I VR 2022victoria tavasÎncă nu există evaluări
- Module 9 - 4 - Circulatory SystemDocument34 paginiModule 9 - 4 - Circulatory SystemThea Shaine B. SILARDEÎncă nu există evaluări
- Fisiologi Cairan Tubuh & Darah: Dr. Nindya Aryanty, M.Med - EdDocument43 paginiFisiologi Cairan Tubuh & Darah: Dr. Nindya Aryanty, M.Med - EdIman TaufiqÎncă nu există evaluări
- Blood Lecture PowerpointDocument116 paginiBlood Lecture Powerpointdrmarybeth100% (3)
- Nurs 107 Blood Physiology Lecture 4Document46 paginiNurs 107 Blood Physiology Lecture 4Ann AgyeiwaaÎncă nu există evaluări
- Blood PDFDocument55 paginiBlood PDFlorrainebarandonÎncă nu există evaluări
- PHS 221 1Document44 paginiPHS 221 1metasynthronos748Încă nu există evaluări
- Hematopoiesis and ErytherokiniticsDocument20 paginiHematopoiesis and ErytherokiniticsShahid F.S.D.Încă nu există evaluări
- Blood Physiology-Lecture 4Document54 paginiBlood Physiology-Lecture 4alfaristurkiÎncă nu există evaluări
- Introd., Haemopoiesis & Plasma ProteinsDocument119 paginiIntrod., Haemopoiesis & Plasma ProteinsShamsuddeen UsmanÎncă nu există evaluări
- 6.2 Human BloodDocument48 pagini6.2 Human BloodSmart ThemisÎncă nu există evaluări
- Blood PhysiologyDocument8 paginiBlood PhysiologypjcaneroÎncă nu există evaluări
- Blood and Blood ComponentsDocument19 paginiBlood and Blood ComponentsMiljun CatacataÎncă nu există evaluări
- University of Guyana Health Sciences FacultyDocument44 paginiUniversity of Guyana Health Sciences FacultySatrohan SurjnarineÎncă nu există evaluări
- Lecture 9 CVSDocument118 paginiLecture 9 CVSMuhammad Abbas WaliÎncă nu există evaluări
- Cardiovascular Physiology 4Document75 paginiCardiovascular Physiology 4maxmus4Încă nu există evaluări
- Haemopoetic SystemDocument73 paginiHaemopoetic SystemManjunathÎncă nu există evaluări
- Blood Lectures 2014 PIO 205Document84 paginiBlood Lectures 2014 PIO 205Philip Abayomi VincentÎncă nu există evaluări
- Ch18 BloodDocument31 paginiCh18 BloodNoah DominoÎncă nu există evaluări
- RBC DISORDERS StudentsDocument84 paginiRBC DISORDERS Studentskimberly abianÎncă nu există evaluări
- Avian Physiology Lecture 003Document36 paginiAvian Physiology Lecture 003Susai Mari NixonÎncă nu există evaluări
- Blood Part 1Document35 paginiBlood Part 1Keziah TampusÎncă nu există evaluări
- Red Blood Cells, Functions, Diseases A Simple Guide To The Condition, Diagnosis, Treatment, And Related ConditionsDe la EverandRed Blood Cells, Functions, Diseases A Simple Guide To The Condition, Diagnosis, Treatment, And Related ConditionsÎncă nu există evaluări
- Fast Facts: Deficiencia de piruvato quinasa para pacientes y familiares: Una enfermedad genética rara que afecta a los glóbulos rojos Información + Asumir el control = El mejor resultadoDe la EverandFast Facts: Deficiencia de piruvato quinasa para pacientes y familiares: Una enfermedad genética rara que afecta a los glóbulos rojos Información + Asumir el control = El mejor resultadoÎncă nu există evaluări
- Without This Message by Purchasing Novapdf : Print To PDFDocument1 paginăWithout This Message by Purchasing Novapdf : Print To PDFvanderphysÎncă nu există evaluări
- 9 Skeletal SystemDocument63 pagini9 Skeletal Systemvanderphys100% (1)
- Study of Microscopic Anatomy - Only 200 Different Cells Types - Four Primary Tissue ClassesDocument61 paginiStudy of Microscopic Anatomy - Only 200 Different Cells Types - Four Primary Tissue ClassesvanderphysÎncă nu există evaluări
- Cells Capable of Shortening & Converting The Chemical Energy of ATP Into Mechanical Energy - Types of Muscle - Physiology of Skeletal MuscleDocument64 paginiCells Capable of Shortening & Converting The Chemical Energy of ATP Into Mechanical Energy - Types of Muscle - Physiology of Skeletal MusclevanderphysÎncă nu există evaluări
- 16 Sense OrgansDocument79 pagini16 Sense OrgansvanderphysÎncă nu există evaluări
- Nucleus and Nucleic Acids - Protein Synthesis and Secretion - DNA Replication and The Cell Cycle - Chromosomes and HeredityDocument53 paginiNucleus and Nucleic Acids - Protein Synthesis and Secretion - DNA Replication and The Cell Cycle - Chromosomes and HeredityvanderphysÎncă nu există evaluări
- Study of Microscopic Anatomy - Only 200 Different Cells Types - Four Primary Tissue ClassesDocument61 paginiStudy of Microscopic Anatomy - Only 200 Different Cells Types - Four Primary Tissue ClassesvanderphysÎncă nu există evaluări
- 600 Human Skeletal Muscles - General Structural & Functional OrganizationDocument61 pagini600 Human Skeletal Muscles - General Structural & Functional OrganizationvanderphysÎncă nu există evaluări
- 14 The Central Nervous SystemDocument61 pagini14 The Central Nervous SystemvanderphysÎncă nu există evaluări
- 8 Bone TissueDocument39 pagini8 Bone Tissuevanderphys100% (1)
- 25 Digestive SystemDocument79 pagini25 Digestive SystemvanderphysÎncă nu există evaluări
- 7 Integumentary SystemDocument38 pagini7 Integumentary Systemvanderphys100% (1)
- 22 Respiratory SystemDocument99 pagini22 Respiratory SystemvanderphysÎncă nu există evaluări
- 25 Digestive SystemDocument79 pagini25 Digestive SystemvanderphysÎncă nu există evaluări
- Evaluation of Global Research Trends in The Area of Food Waste D - 2020 - Food CDocument10 paginiEvaluation of Global Research Trends in The Area of Food Waste D - 2020 - Food CAliÎncă nu există evaluări
- 300.91C - Fire Alarm System Pre-Test and Acceptance Test Checklist 3-27-14Document2 pagini300.91C - Fire Alarm System Pre-Test and Acceptance Test Checklist 3-27-14mthuyaÎncă nu există evaluări
- Philips Family Lamp UV CDocument4 paginiPhilips Family Lamp UV CmaterpcÎncă nu există evaluări
- Ar ExportsDocument1 paginăAr ExportsRais AlamÎncă nu există evaluări
- Tsang Mui Millennium School 2019-2020 English Worksheet: Fill in The Blanks With The Correct Form of The VerbsDocument46 paginiTsang Mui Millennium School 2019-2020 English Worksheet: Fill in The Blanks With The Correct Form of The VerbscocoyipÎncă nu există evaluări
- MicrosoftDynamicsNAVAdd OnsDocument620 paginiMicrosoftDynamicsNAVAdd OnsSadiq QudduseÎncă nu există evaluări
- Watercolor SecretsDocument60 paginiWatercolor Secretsmissdoisneau98% (47)
- Hydrostatic, Deviatoric StressesDocument7 paginiHydrostatic, Deviatoric StressespanbuÎncă nu există evaluări
- DuctBank For Electrical SystemDocument4 paginiDuctBank For Electrical SystemAnonymous XYAPaxjbYÎncă nu există evaluări
- Chapter 1 Cumulative Review: Multiple ChoiceDocument2 paginiChapter 1 Cumulative Review: Multiple ChoiceJ. LeeÎncă nu există evaluări
- Moving Money Box: Pig (Assembly Instructions) : The Movements Work Better With Heavier CoinsDocument6 paginiMoving Money Box: Pig (Assembly Instructions) : The Movements Work Better With Heavier CoinsjuanÎncă nu există evaluări
- 19 Free Amigurumi Crochet Patterns: MaterialsDocument4 pagini19 Free Amigurumi Crochet Patterns: MaterialsLucica Diaconu100% (1)
- Long Quiz 1 Eim Tools, MaterialsDocument1 paginăLong Quiz 1 Eim Tools, MaterialsLea Ann PalaciosÎncă nu există evaluări
- Beauty Therapy Thesis SampleDocument8 paginiBeauty Therapy Thesis Samplerachelvalenzuelaglendale100% (2)
- TSBDocument3 paginiTSBnoe dela vegaÎncă nu există evaluări
- Oc818 Manual v03-1Document5 paginiOc818 Manual v03-1Luca PayetÎncă nu există evaluări
- Cooking Off The Clock by Elizabeth Falkner - Recipes and ExcerptDocument16 paginiCooking Off The Clock by Elizabeth Falkner - Recipes and ExcerptThe Recipe ClubÎncă nu există evaluări
- Saberon StratMan2Document3 paginiSaberon StratMan2paredesladyheart18Încă nu există evaluări
- UNDP NP Dhangadhi SWM TOR FinalDocument4 paginiUNDP NP Dhangadhi SWM TOR FinalNirmal K.c.Încă nu există evaluări
- Air Cooler With Checking DoorDocument2 paginiAir Cooler With Checking DoorSuraj KumarÎncă nu există evaluări
- Toda People in IndiaDocument9 paginiToda People in IndiaAmoona KopiKoÎncă nu există evaluări
- (Q2) Electrochemistry 29th JulyDocument21 pagini(Q2) Electrochemistry 29th JulySupritam KunduÎncă nu există evaluări
- NMMT City Bus SystemDocument3 paginiNMMT City Bus Systemharish guptaÎncă nu există evaluări
- Lesson 2 Arts of East AsiaDocument21 paginiLesson 2 Arts of East Asiarenaldo ocampoÎncă nu există evaluări
- Unit Test 7 (PDF)Document1 paginăUnit Test 7 (PDF)emirelliucÎncă nu există evaluări
- De Thi Vao 10 Chuyen Hoa Nguyen Trai Hai Duong 20212022Document2 paginiDe Thi Vao 10 Chuyen Hoa Nguyen Trai Hai Duong 20212022Trần Ngọc BíchÎncă nu există evaluări
- Sunday Afternoon, October 27, 2013: TechnologyDocument283 paginiSunday Afternoon, October 27, 2013: TechnologyNatasha MyersÎncă nu există evaluări
- Carriages and Mounts SeriesDocument92 paginiCarriages and Mounts Seriessudhirm16Încă nu există evaluări
- Iec TR 62343-6-8-2011Document14 paginiIec TR 62343-6-8-2011Amer AmeryÎncă nu există evaluări
- Vision For Mobile Robot Navigation - A Survey PDFDocument31 paginiVision For Mobile Robot Navigation - A Survey PDFtes donlodÎncă nu există evaluări