Documente Academic
Documente Profesional
Documente Cultură
Anticancer
Încărcat de
enterprenuer cel0 evaluări0% au considerat acest document util (0 voturi)
49 vizualizări15 paginiTitlu original
anticancer.ppt.pptx
Drepturi de autor
© © All Rights Reserved
Formate disponibile
PPTX, PDF, TXT sau citiți online pe Scribd
Partajați acest document
Partajați sau inserați document
Vi se pare util acest document?
Este necorespunzător acest conținut?
Raportați acest documentDrepturi de autor:
© All Rights Reserved
Formate disponibile
Descărcați ca PPTX, PDF, TXT sau citiți online pe Scribd
0 evaluări0% au considerat acest document util (0 voturi)
49 vizualizări15 paginiAnticancer
Încărcat de
enterprenuer celDrepturi de autor:
© All Rights Reserved
Formate disponibile
Descărcați ca PPTX, PDF, TXT sau citiți online pe Scribd
Sunteți pe pagina 1din 15
Anticancer drugs
Cancer is a disease characterised by uncontrolled
multiplication and spread of abnormal forms of the body's
own cells.
The terms cancer, malignant neoplasm (neoplasm simply
means 'new growth') and malignant tumour are synonymous.
Both benign and malignant tumours manifest uncontrolled
proliferation, but the latter are distinguished by their capacity
for dedifferentiation, their invasiveness and their ability
to metastasise (spread to other parts of the body).
The appearance of these abnormal characteristics reflects
altered patterns of gene expression in the cancer cells,
resulting from genetic mutations.
There are three main approaches to treating
established cancer-
surgical excision,
irradiation
Chemotherapy
The relative value of each of these approaches depends on the
type of tumour and the stage of its development.
Chemotherapy may be used on its own or as an adjunct to other
forms of therapy.
THE PATHOGENESIS OF CANCER
Cancer cells manifest, to varying degrees,
four characteristics that distinguish them
from normal cells.
These are
uncontrolled proliferation
dedifferentiation and loss of function
invasiveness
metastasis.
THE GENESIS OF A CANCER CELL
Normal cell turns into a cancer cell because of one or more
mutations in its DNA, which can be acquired or inherited.
A good example is breast cancer; women who inherit a
single defective copy of either of the tumour suppressor
genes BRCA1 and BRCA2 have a significantly increased
risk of developing breast cancer.
However, carcinogenesis is a complex multistage process,
usually involving more than one genetic change as well as
other, epigenetic factors (hormonal, cocarcinogen and
tumour promoter effects, etc.) that do not themselves
produce cancer but which increase the likelihood that the
genetic mutation(s) will result eventually result in cancer.
There are two main categories of genetic change
that are important.
The activation of proto-oncogenes to
oncogenes.
Proto-oncogenes are genes that normally control cell division,
apoptosis and differentiation, but which can be converted to
oncogenes that induce malignant change by viral or
carcinogen action.
The inactivation of tumour suppressor
genes.
Normal cells contain genes that have the ability to suppress
malignant change-termed tumour suppressor genes
(antioncogenes)-and there is now good evidence that
mutations of these genes are involved in many different
cancers. The loss of function of tumour suppressor genes can
be the critical event in carcinogenesis.
Alkylating agents and related compounds,
Nitrogen mustards (Mechlorethamine , Cyclophosphamide, Ifosfamide,Melphalan
(L-sarcolysin), Chlorambucil)
Ethyleneimines and methylmelamines (Altretamine, Thiotepa)
Methylhydrazine derivative(Procarbazine)
Alkyl sulfonate(Busulfan)
Nitrosoureas(Carmustine, Streptozocin (streptozotocin))
Triazenes (Dacarbazine )
Platinum coordination complexes (Cisplatin, carboplatin,oxaliplatin)
antimetabolites,
Folic acid analogs Methotrexate (amethopterin)
Pyrimidine analogs( Fluorouracil, capecitabine, Cytarabine, Gemcitabine.
Purine analogs and related inhibitors (6-mercaptopurinePentostatin)
Cytotoxic antibiotics (bleomycin, Doxorubucin, Daunorubucin, idarubicin,
Dactinomycin)
plant derivatives (vinca alkaloids, taxanes, campothecins)
Hormones (Adrenocortical suppressants, Adrenocorticosteroids,
Progestins, Estrogens, Anti-estrogens, Aromatase inhibitors,
Androgens, Anti-androgen, Gonadotropin-releasing hormone analog
Miscellaneous agents (Tretinoin, arsenic trioxide, Imatinib,
Gefitinib, erlotinib)
undergoes intramolecular
cyclisation, forming an
unstable ethylene
immonium cation (2) and
releasing Cl-, the tertiary
amine being transformed to
a quaternary ammonium
compound. The strained
ring of the ethylene
immonium intermediate
opens to form a reactive
carbonium ion (in yellow
box) (3), which reacts
immediately with N7 of
guanine (in green circle) to
give 7-alkylguanine (bond
shown in blue), the N7
being converted to a
quaternary ammonium
nitrogen. These reactions
can then be repeated with
thea other
Alkylation and cross-linking of DNA by -CH2mustard
nitrogen CH2Cl to give
a cross-link.
The metabolism of
cyclophosphamide.
Cyclophosphamide is
inactive until
metabolised in the
liver by P450 mixed
function oxidases to
4-
hydroxycyclophospha
mide, which
(reversibly) forms
aldophosphamide.
Aldophosphamide is
conveyed to other
tissues, where it is
converted to
phosphoramide
mustard, the actual
cytotoxic molecule,
and acrolein, which is
responsible for
unwanted effects.
The part of the
cyclophosphamide
molecule that gives
rise to the active
metabolites is shown
in the blue box.
S-ar putea să vă placă și
- Biology: a QuickStudy Laminated Reference GuideDe la EverandBiology: a QuickStudy Laminated Reference GuideEvaluare: 3 din 5 stele3/5 (2)
- Sustainable synthesis of ciclopentene derivatives through multicomponent reactions in continuous flow regimeDe la EverandSustainable synthesis of ciclopentene derivatives through multicomponent reactions in continuous flow regimeÎncă nu există evaluări
- On Agents of MutationDocument22 paginiOn Agents of Mutationmine_ne361Încă nu există evaluări
- Between The Newly Synthesized Strand and The Template StrandDocument52 paginiBetween The Newly Synthesized Strand and The Template StrandAdith SaiÎncă nu există evaluări
- Anticancer Drugs NotesDocument112 paginiAnticancer Drugs Notesdnyanshri bhamareÎncă nu există evaluări
- Lecture 5 PharmacotoxicologyDocument19 paginiLecture 5 Pharmacotoxicologykeishini2001Încă nu există evaluări
- Molecular Mechanism of MutationsDocument38 paginiMolecular Mechanism of MutationsAnirudh Acharya100% (6)
- Anticancer Drugs Med ChemDocument215 paginiAnticancer Drugs Med ChemCurex QAÎncă nu există evaluări
- Anti Neoplastic AgentsDocument23 paginiAnti Neoplastic AgentsHawkar QadirÎncă nu există evaluări
- Antineoplastic AgentsDocument10 paginiAntineoplastic AgentsMuhamed ArsalanÎncă nu există evaluări
- Dna Mutation & Repair MechanismDocument23 paginiDna Mutation & Repair MechanismOsama Bin RizwanÎncă nu există evaluări
- Conventional Anticancer Chemotherapy Part 1Document57 paginiConventional Anticancer Chemotherapy Part 1Jia YingÎncă nu există evaluări
- ANTIMALARIALSDocument24 paginiANTIMALARIALSjou joÎncă nu există evaluări
- Antimalarial DrugsDocument5 paginiAntimalarial DrugsjtuyishiÎncă nu există evaluări
- Anti Cancer Drugs...Document62 paginiAnti Cancer Drugs...KwirimeÎncă nu există evaluări
- Question 2Document26 paginiQuestion 2garybee37Încă nu există evaluări
- AnticancerDocument19 paginiAnticancerKabirÎncă nu există evaluări
- Alkylating AgentsDocument53 paginiAlkylating AgentsDhanya KcÎncă nu există evaluări
- AnticancerDocument38 paginiAnticancerSuman ChauhanÎncă nu există evaluări
- Parasympathomimetics and ParasympatholyticsDocument16 paginiParasympathomimetics and ParasympatholyticsSalona Roy100% (4)
- Gene Mutation: Genomes 3Document72 paginiGene Mutation: Genomes 3Abdus SubhanÎncă nu există evaluări
- Antikanker S1-IvcDocument72 paginiAntikanker S1-IvcNina RishantiÎncă nu există evaluări
- AnticancerDocument27 paginiAnticancerLoreine Jane ClaritoÎncă nu există evaluări
- All Anticacer DrugsDocument7 paginiAll Anticacer DrugsDrMadhu AdusumilliÎncă nu există evaluări
- (Biochemistry) Onsite Assignment No8 - Group XDocument33 pagini(Biochemistry) Onsite Assignment No8 - Group XV THÎncă nu există evaluări
- Alkylating Agents and Related DrugsDocument35 paginiAlkylating Agents and Related Drugsgrace caasiÎncă nu există evaluări
- 112 Anti Neoplastic AgentsDocument4 pagini112 Anti Neoplastic AgentsJC LumayaÎncă nu există evaluări
- Chemico-Biological Interactions: SciencedirectDocument11 paginiChemico-Biological Interactions: SciencedirectDánica Nicoll Rojas MolinaÎncă nu există evaluări
- Alkylating AgentsDocument3 paginiAlkylating AgentsIna SimacheÎncă nu există evaluări
- AnticancerDocument5 paginiAnticancerAiman TymerÎncă nu există evaluări
- D. Types of MutationDocument11 paginiD. Types of MutationDeepali SinghÎncă nu există evaluări
- Alkyating AgentsDocument21 paginiAlkyating Agentsaditikaushik2006Încă nu există evaluări
- The Replication of DNA: NiveditaDocument53 paginiThe Replication of DNA: NiveditaLalruatdiki CÎncă nu există evaluări
- Herbal Drug and ChemistryDocument67 paginiHerbal Drug and ChemistrymayankÎncă nu există evaluări
- Anticancer DrugsDocument27 paginiAnticancer DrugsAnupamÎncă nu există evaluări
- Anticancer Drugs: Dr. R. Jamuna Rani MD, Professor & Hod Dept. of PharmacologyDocument69 paginiAnticancer Drugs: Dr. R. Jamuna Rani MD, Professor & Hod Dept. of PharmacologyMarlindah SÎncă nu există evaluări
- DNA Mutation Workshop GuideDocument7 paginiDNA Mutation Workshop GuideGio GallegoÎncă nu există evaluări
- Soal UabDocument21 paginiSoal UabCynthiaÎncă nu există evaluări
- Review Article: Imatinib: A Breakthrough of Targeted Therapy in CancerDocument10 paginiReview Article: Imatinib: A Breakthrough of Targeted Therapy in CancerMohammad AdhinÎncă nu există evaluări
- Carcinogen e IsDocument108 paginiCarcinogen e IsIndranil GhoshÎncă nu există evaluări
- DNA Damage and RepairDocument32 paginiDNA Damage and RepairNashmiya SaheerÎncă nu există evaluări
- MUTATIONDocument9 paginiMUTATIONNorisah NirishÎncă nu există evaluări
- Mutation and RepairDocument42 paginiMutation and RepairGracia NataliaÎncă nu există evaluări
- CH11-Amino Acid MetabolismDocument106 paginiCH11-Amino Acid MetabolismChatchawinÎncă nu există evaluări
- Genetic Material-DNA: 6 November 2003 Reading:The Cell Chapter 5, Pages: 192-201Document38 paginiGenetic Material-DNA: 6 November 2003 Reading:The Cell Chapter 5, Pages: 192-201Laura VgÎncă nu există evaluări
- Anticancer 1 P2Document4 paginiAnticancer 1 P2N Gv FcÎncă nu există evaluări
- Chemistry of DNA Damage RepairDocument11 paginiChemistry of DNA Damage RepairazzaassÎncă nu există evaluări
- Biological Membranes & TransportDocument58 paginiBiological Membranes & TransportShimmering MoonÎncă nu există evaluări
- Cancer Chemotherapy by MaryamDocument51 paginiCancer Chemotherapy by MaryammaryamÎncă nu există evaluări
- Xanthone Journal PDFDocument12 paginiXanthone Journal PDFftrynÎncă nu există evaluări
- GeneticsDocument25 paginiGeneticsAnanya SinghÎncă nu există evaluări
- Anticancer Agents Dr. Nutan RaoDocument40 paginiAnticancer Agents Dr. Nutan RaoRahul LokhandeÎncă nu există evaluări
- Antimalarial Drugs History, New Antimalarial Drugs and Antimalarial Vaccines MalariaDocument9 paginiAntimalarial Drugs History, New Antimalarial Drugs and Antimalarial Vaccines MalariainzemamÎncă nu există evaluări
- Anti-Neoplastic Agents 1Document76 paginiAnti-Neoplastic Agents 1Soubia AamirÎncă nu există evaluări
- Lecture 5 DNA Mutation and DNA Repair-2Document65 paginiLecture 5 DNA Mutation and DNA Repair-2Constance WongÎncă nu există evaluări
- Acetate, Mevalonate and Shikimic Acid PathwaysDocument19 paginiAcetate, Mevalonate and Shikimic Acid Pathwaysamitaggarwal7888% (8)
- BioChem I Lecture Notes - Parth GDocument72 paginiBioChem I Lecture Notes - Parth GParthian ComicsÎncă nu există evaluări
- Anti Cancer DrugsDocument56 paginiAnti Cancer DrugsTimothy David50% (2)
- Total Synthesis of Angel Mar inDocument4 paginiTotal Synthesis of Angel Mar inRafael GalloÎncă nu există evaluări
- Anticancer DrugDocument29 paginiAnticancer DrugAnjana PaudelÎncă nu există evaluări
- GATE 2018 Electrical Engineering 10-02-2018 Afternoon Session Detailed SolutionDocument43 paginiGATE 2018 Electrical Engineering 10-02-2018 Afternoon Session Detailed SolutionDebajyoti DattaÎncă nu există evaluări
- Tutorial PDFDocument68 paginiTutorial PDFOsmar BorgesÎncă nu există evaluări
- Chap 11Document41 paginiChap 11mahawebÎncă nu există evaluări
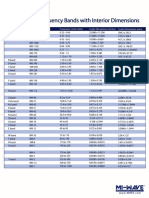
- Waveguide ChartDocument1 paginăWaveguide Chartenterprenuer celÎncă nu există evaluări
- Notes4 Sparams PDFDocument20 paginiNotes4 Sparams PDFaozgurluk_scribdÎncă nu există evaluări
- Caspers S ParametersDocument54 paginiCaspers S ParametersArvind SrivastavaÎncă nu există evaluări
- Hospital PharmacyDocument32 paginiHospital Pharmacyenterprenuer celÎncă nu există evaluări
- AnticancerDocument15 paginiAnticancerenterprenuer celÎncă nu există evaluări