Documente Academic
Documente Profesional
Documente Cultură
Periodontology MCQ
Încărcat de
Mohamad Said0 evaluări0% au considerat acest document util (0 voturi)
171 vizualizări103 paginiPERIODONTOLOGY
Titlu original
PERIODONTOLOGY MCQ
Drepturi de autor
© © All Rights Reserved
Formate disponibile
PPT, PDF, TXT sau citiți online pe Scribd
Partajați acest document
Partajați sau inserați document
Vi se pare util acest document?
Este necorespunzător acest conținut?
Raportați acest documentPERIODONTOLOGY
Drepturi de autor:
© All Rights Reserved
Formate disponibile
Descărcați ca PPT, PDF, TXT sau citiți online pe Scribd
0 evaluări0% au considerat acest document util (0 voturi)
171 vizualizări103 paginiPeriodontology MCQ
Încărcat de
Mohamad SaidPERIODONTOLOGY
Drepturi de autor:
© All Rights Reserved
Formate disponibile
Descărcați ca PPT, PDF, TXT sau citiți online pe Scribd
Sunteți pe pagina 1din 103
Oral Pathology
Chapter 17
Copyright © 2005 by Elsevier Inc. All rights reserved.
Introduction
Oral pathology is the study of
diseases in the oral cavity.
Only a dentist or physician may diagnose
pathologic (disease) conditions, but it is
important for the dental assistant to be
able to recognize the differences between
normal and abnormal conditions that
appear in the mouth.
Copyright © 2005 by Elsevier Inc. All rights reserved.
Terminology Used to Describe Oral Lesions
• Lesion is a broad term for abnormal tissues in the
oral cavity that includes wounds, sores, and any
other tissue damage caused by injury or disease.
• Determining the type of lesion in a disease is one of
the earliest steps in formulating a differential
diagnosis.
• Types of lesions of the oral mucosa are classified as
to whether they:
– Extend below or extend above the surface.
– Are flat or even with the surface.
Copyright © 2005 by Elsevier Inc. All rights reserved.
• Many systemic diseases as well as infectious
diseases have oral manifestations
(signs and symptoms).
• The dental assistant should also understand how
oral abnormalities affect the patient’s general health
and planned dental treatment.
• Before you can recognize the abnormal conditions,
you must have a solid understanding of the
appearance of the normal oral conditions.
Copyright © 2005 by Elsevier Inc. All rights reserved.
Lesions Extending Below the Surface
• Ulcer: A defect or break in continuity of the mucosa
that creates a punched-out area similar to a crater.
• Erosion of the soft tissue: A shallow defect in the
mucosa caused by mechanical trauma.
• Abscess: A localized collection of pus in a
circumscribed area.
• Cyst: A closed sac or pouch that is lined with
epithelium and contains fluid or semisolid material.
Copyright © 2005 by Elsevier Inc. All rights reserved.
• The dental assistant should understand the terms
used to describe pathologic conditions and record
preliminary identification and descriptions of lesions.
• You should use these terms in the clinical setting so
that they become part of your everyday professional
vocabulary.
• You then can communicate effectively with
other professionals.
Copyright © 2005 by Elsevier Inc. All rights reserved.
Lesions Extending Above the Surface
• Blisters: Also known as vesicles, lesions filled
with a watery fluid.
• Pustule: Similar in appearance to a blister, but it
contains pus.
• Hematoma: Also similar to a blister, but it
contains blood.
• Plaque: Any patch or flat area that is slightly
raised from the surface.
Copyright © 2005 by Elsevier Inc. All rights reserved.
Sources of Information for Diagnosis
• Historical
• Clinical
• Radiographic
• Laboratory
• Microscopic
• Surgical
• Therapeutic
• Differential findings
Copyright © 2005 by Elsevier Inc. All rights reserved.
Historical Information
• Family histories are important because of
genetic disorders such as dentinogenesis
imperfecta
• Melanin pigmentation of the gingiva is
common in dark-skinned individuals.
Copyright © 2005 by Elsevier Inc. All rights reserved.
Fig. 17-1 Dentinogenesis imperfecta
(From Ibsen OC, Phelan JA: Oral pathology for the dental hygienist, ed 4, St. Louis, 2004, Saunders.)
Copyright © 2005 by Elsevier Inc. All rights reserved.
Fig. 17-2 Melanin pigmentation
(From Ibsen OC, Phelan JA: Oral pathology for the dental hygienist, ed 4, St. Louis, 2004, Saunders.)
Copyright © 2005 by Elsevier Inc. All rights reserved.
Examples Of Conditions Diagnosed
On The Basis Of Clinical Appearance
• Fissured tongue
• Maxillary and mandibular tori
• Median rhomboid glossitis
Copyright © 2005 by Elsevier Inc. All rights reserved.
Fig. 17-3 Fissured tongue
(From Ibsen OC, Phelan JA: Oral pathology for the dental hygienist, ed 4, St. Louis, 2004, Saunders.)
Copyright © 2005 by Elsevier Inc. All rights reserved.
Fig. 17-4 A, Clinical appearance of bilateral mandibular tori
(From Ibsen OC, Phelan JA: Oral pathology for the dental hygienist, ed 4, St. Louis, 2004, Saunders.)
Copyright © 2005 by Elsevier Inc. All rights reserved.
Fig. 17-4 B, Clinical appearance of lobulated torus palatinus
(From Ibsen OC, Phelan JA: Oral pathology for the dental hygienist, ed 4, St. Louis, 2004, Saunders.)
Copyright © 2005 by Elsevier Inc. All rights reserved.
Fig. 17-5 Median rhomboid glossitis
(From Ibsen OC, Phelan JA: Oral pathology for the dental hygienist, ed 4, St. Louis, 2004, Saunders.)
Copyright © 2005 by Elsevier Inc. All rights reserved.
Radiographs
• Excellent in providing information about:
– Periapical pathology
– Internal resorption
– Impacted teeth
Copyright © 2005 by Elsevier Inc. All rights reserved.
Fig. 17-6 Periapical pathology
(From Ibsen OC, Phelan JA: Oral pathology for the dental hygienist, ed 4, St. Louis, 2004, Saunders.)
Copyright © 2005 by Elsevier Inc. All rights reserved.
Fig. 17-7 Internal resorption
(From Ibsen OC, Phelan JA: Oral pathology for the dental hygienist, ed 4, St. Louis, 2004, Saunders.)
Copyright © 2005 by Elsevier Inc. All rights reserved.
Fig. 17-8 Horizontal impaction of the third molar
(From Ibsen OC, Phelan JA: Oral pathology for the dental hygienist, ed 4, St. Louis, 2004, Saunders.)
Copyright © 2005 by Elsevier Inc. All rights reserved.
Microscopic Diagnosis
• When a suspicious lesion is present, tissue is
removed and sent to a pathology laboratory
where it is evaluated microscopically (biopsy).
• This procedure is very often used to make the
definitive (final) diagnosis.
• For example, a white lesion cannot be diagnosed
on the basis of the clinical appearance alone.
It must have a biopsy to determine if it is
malignant or not .
Copyright © 2005 by Elsevier Inc. All rights reserved.
Fig. 17-9 A white lesion is seen on the anterior
floor and ventral surface of the tongue.
(From Ibsen OC, Phelan JA: Oral pathology for the dental hygienist, ed 4, St. Louis, 2004, Saunders.)
Copyright © 2005 by Elsevier Inc. All rights reserved.
Therapeutic Diagnosis
• Therapeutic diagnosis is made by providing a
treatment (therapy), then seeing how the condition
responds. For example, angular cheilitis could be
caused by a lack of the B-complex vitamins.
• It could simply be a fungal infection.
• If the angular cheilitis improved after the patient
was given an antifungal cream, the vitamin
deficiency theory could be ruled out.
Copyright © 2005 by Elsevier Inc. All rights reserved.
Fig. 17-10 Angular cheilitis
(From Ibsen OC, Phelan JA: Oral pathology for the dental hygienist, ed 4, St. Louis, 2004, Saunders.)
Copyright © 2005 by Elsevier Inc. All rights reserved.
Surgical Diagnosis
• A diagnosis is made based on the findings from a
surgical procedure.
– For example, on a radiograph a traumatic bone
cyst also looks like a static bone cyst.
• However, one condition would require treatment,
one would not. Surgically opening the area and
inspecting the area would prove if the radiolucency
on the radiograph was indeed a condition that
needed further treatment or not.
Copyright © 2005 by Elsevier Inc. All rights reserved.
Fig. 17-11 Traumatic bone cyst
(Courtesy Dr. Edward V. Zegarelli. From Ibsen OC, Phelan JA: Oral pathology for the dental hygienist, ed 4, St. Louis, 2004, Saunders.)
Copyright © 2005 by Elsevier Inc. All rights reserved.
Fig. 17-12 Arrow points to static bone cyst
(Courtesy Dr. Edward V. Zegarelli. From Ibsen OC, Phelan JA: Oral pathology for the dental hygienist, ed 4, St. Louis, 2004, Saunders.)
Copyright © 2005 by Elsevier Inc. All rights reserved.
Diseases of the Oral Soft
Tissues
Copyright © 2005 by Elsevier Inc. All rights reserved.
Leukoplakia
• Leukoplakia means white patch.
• Lesions vary in appearance and texture from a fine
white transparency to a heavy, thick, warty plaque.
• The cause is unknown but is commonly linked to
chronic irritation or trauma.
• Leukoplakia very often precedes the development
of a malignant tumor.
Copyright © 2005 by Elsevier Inc. All rights reserved.
Fig. 17-14 Leukoplakia
(From Ibsen OC, Phelan JA: Oral pathology for the dental hygienist, ed 4, St. Louis, 2004, Saunders.)
Copyright © 2005 by Elsevier Inc. All rights reserved.
Lichen Planus
• A benign, chronic disease affecting the skin
and oral mucosa.
• Many factors have been implicated in lichen
planus; however, the cause remains unknown.
• On the oral mucosa, the patchy white lesions
have a characteristic pattern of circles and
interconnecting lines called Wickham's striae.
Copyright © 2005 by Elsevier Inc. All rights reserved.
Fig. 17-15 Lichen planus
(From Ibsen OC, Phelan JA: Oral pathology for the dental hygienist, ed 4, St. Louis, 2004, Saunders.)
Copyright © 2005 by Elsevier Inc. All rights reserved.
Candidiasis
• A superficial infection caused by the yeastlike
fungus, Candida albicans.
• Candidiasis does occur under conditions such as
antibiotic therapy, diabetes, xerostomia (dry mouth),
and weakened immunologic reactions.
• It can be the initial clinical manifestation for patients
with acquired immunodeficiency syndrome (AIDS).
• Diaper rash, vaginitis, and thrush are also common
types of candidiasis.
Copyright © 2005 by Elsevier Inc. All rights reserved.
Types of Candidiasis
• Pseudomembranous candidiasis: thrush
• Hyperplastic candidiasis
• Atrophic candidiasis
Copyright © 2005 by Elsevier Inc. All rights reserved.
Fig. 17-16 Pseudomembranous candidiasis
(From Ibsen OC, Phelan JA: Oral pathology for the dental hygienist, ed 4, St. Louis, 2004, Saunders.)
Copyright © 2005 by Elsevier Inc. All rights reserved.
Fig. 17-17 Chronic hyperplastic candidiasis. The white appearance of the
tongue did not wipe off, and it disappeared with antifungal treatment.
(From Ibsen OC, Phelan JA: Oral pathology for the dental hygienist, ed 4, St. Louis, 2004, Saunders.)
Copyright © 2005 by Elsevier Inc. All rights reserved.
Aphthous Ulcers
• Aphthous ulcers are also known as aphthous
stomatitis or canker sores.
• Recurrent aphthous ulcers (RAU) is a disease that
causes recurring outbreaks of blister-like sores
inside the mouth and on the lips.
– Minor RAU: Episodes fewer than six times a year;
lesions usually heal within 7 to 10 days.
– Major RAU: Outbreaks of larger, deeper ulcers
that take longer to heal.
Copyright © 2005 by Elsevier Inc. All rights reserved.
Fig. 17-18 Minor aphthous ulcer
(From Ibsen OC, Phelan JA: Oral pathology for the dental hygienist, ed 4, St. Louis, 2004, Saunders.)
Copyright © 2005 by Elsevier Inc. All rights reserved.
Cellulitis
• Inflammation spreads through the soft tissue
or organ.
• Swelling develops rapidly, with a high fever.
• The skin becomes very red, and there is
severe throbbing pain as the inflammation
localizes.
• Cellulitis associated with oral infections is
potentially dangerous because it can travel
quickly to sensitive tissues such as the eye
or brain.
Copyright © 2005 by Elsevier Inc. All rights reserved.
Fig. 17-19 Cellulitis
(From Ibsen OC, Phelan JA: Oral pathology for the dental hygienist, ed 4, St. Louis, 2004, Saunders.)
Copyright © 2005 by Elsevier Inc. All rights reserved.
Conditions of
the Tongue
Copyright © 2005 by Elsevier Inc. All rights reserved.
Glossitis
Glossitis is the general term used to describe
inflammation and changes in the topography of
the tongue.
Copyright © 2005 by Elsevier Inc. All rights reserved.
Black Hairy Tongue
• Black hairy tongue may be caused by the oral flora
imbalance after the administration of antibiotics.
• The filiform papillae are so greatly elongated that
they resemble hairs.
• These elongated papillae become stained by food
and tobacco, producing the name black hairy tongue.
Copyright © 2005 by Elsevier Inc. All rights reserved.
Fig. 17-20 Black hairy tongue
(From Ibsen OC, Phelan JA: Oral pathology for the dental hygienist, ed 4, St. Louis, 2004, Saunders.)
Copyright © 2005 by Elsevier Inc. All rights reserved.
Geographic Tongue
• The tongue develops multiple areas of desquamation
(loss) of the filiform papillae in several irregularly
shaped but well-demarcated areas.
• The smooth areas resemble a map, thus the name
geographic tongue.
• Over a period of days or weeks, the smooth areas
and the whitish margins seem to migrate across the
surface of the tongue by healing on one border and
extending on another.
Copyright © 2005 by Elsevier Inc. All rights reserved.
Fig. 17-21 Geographic tongue
(From Ibsen OC, Phelan JA: Oral pathology for the dental hygienist, ed 4, St. Louis, 2004, Saunders.)
Copyright © 2005 by Elsevier Inc. All rights reserved.
Fissured Tongue
• A variant of normal; its cause is unknown.
• Some theories include a vitamin deficiency or
chronic trauma over a long period.
• The dorsal surface (top) of the tongue appears to
have deep fissures or grooves that become irritated
if food debris collects in them.
• The patient with a fissured tongue is advised to
brush the tongue gently with a soft toothbrush to
keep the fissures clean of debris and irritants.
Copyright © 2005 by Elsevier Inc. All rights reserved.
Fig. 17-22 Fissured tongue
(From Ibsen OC, Phelan JA: Oral pathology for the dental hygienist, ed 4, St. Louis, 2004, Saunders.)
Copyright © 2005 by Elsevier Inc. All rights reserved.
Pernicious Anemia
• Pernicious anemia is a condition in which the body
does not absorb vitamin B12.
• People who have this condition show signs of anemia,
weakness, pallor, and fatigue on exertion.
• Other signs can include nausea, diarrhea, abdominal
pain, and loss of appetite.
• The oral manifestations of pernicious anemia include
angular cheilitis (ulceration and redness at the corners
of the lips), mucosal ulceration, loss of papillae on the
tongue, and a burning and painful tongue.
Copyright © 2005 by Elsevier Inc. All rights reserved.
Fig. 17-23 Iron deficiency. The tongue is devoid of filiform papillae.
Angular cheilitis was also present in this patient.
(From Ibsen OC, Phelan JA: Oral pathology for the dental hygienist, ed 4, St. Louis, 2004, Saunders.)
Copyright © 2005 by Elsevier Inc. All rights reserved.
Oral Cancer
Copyright © 2005 by Elsevier Inc. All rights reserved.
Oral Cancer
• Oral cancer is one of the 10 most frequently
occurring cancers in the world.
• The incidence, as well as the site, of the cancer
varies greatly from country to country. In the Western
countries, the site most often affected is the
vermilion border of the lip.
• Most oral cancers do not cause pain in the early
stages, and the thorough dentist is most likely to be
the first to detect them. These cancers are fatal if not
detected early enough or if left untreated.
Copyright © 2005 by Elsevier Inc. All rights reserved.
Fig. 17-24 Squamous cell carcinoma of the lower lip
(From Ibsen OC, Phelan JA: Oral pathology for the dental hygienist, ed 4, St. Louis, 2004, Saunders.)
Copyright © 2005 by Elsevier Inc. All rights reserved.
Types of Oral Cancer
• A carcinoma is a malignant neoplasm (growth) of the
epithelium (tissue lining the mouth).
• An adenocarcinoma is a malignant tumor that arises from
the submucous glands underlying the oral mucosa.
• A sarcoma is a malignant neoplasm arising from supportive
and connective tissue.
• An osteosarcoma is a malignant tumor involving the bone.
In the mouth, the affected bones are the bones of the jaws.
Although the cancer may start in the bone, it often spreads
and involves the surrounding soft tissues.
Copyright © 2005 by Elsevier Inc. All rights reserved.
Fig. 17-25 Panoramic radiograph showing destruction
of the mandible by squamous cell carcinoma
(From Ibsen OC, Phelan JA: Oral pathology for the dental hygienist, ed 4, St. Louis, 2004, Saunders.)
Copyright © 2005 by Elsevier Inc. All rights reserved.
Leukemia
• A cancer of the blood-forming organs that is
characterized by rapid growth of immature white
blood cells.
• Oral symptoms of leukemia may be some of the first
indications of the disease.
• Symptoms in the gingival tissues include
hemorrhage, ulceration, enlargement, spongy
texture, and magenta coloration of the gingiva.
• Enlargement of lymph nodes, symptoms of anemia,
and general bleeding tendencies are typical.
Copyright © 2005 by Elsevier Inc. All rights reserved.
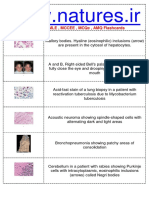
Fig. 17-26 Leukemia
(From Ibsen OC, Phelan JA: Oral pathology for the dental hygienist, ed 4, St. Louis, 2004, Saunders.)
Copyright © 2005 by Elsevier Inc. All rights reserved.
Smokeless Tobacco
• Chewing tobacco or snuff presents a serious
health hazard.
• It is a major concern because of the high rates of
precancerous leukoplakia and oral cancer occurring
among users of smokeless tobacco.
• Cancers of the pharynx, larynx, and esophagus
occur 400 to 500 times more frequently.
• Smokeless tobacco is also linked to an increased
incidence of tooth loss from periodontal disease.
Copyright © 2005 by Elsevier Inc. All rights reserved.
Fig. 17-27 Tobacco chewer’s white lesion.
Note the rough texture of the surface.
(From Ibsen OC, Phelan JA: Oral pathology for the dental hygienist, ed 4, St. Louis, 2004, Saunders.)
Copyright © 2005 by Elsevier Inc. All rights reserved.
Dental Implications of Radiation Therapy
• Xerostomia: Lack of adequate saliva and the reduced
blood supply can cause oral infections, delay
healing, and make it very difficult to wear dentures.
• Radiation caries: Caused by the lack of saliva,
usually appear first in the cervical areas of the teeth.
The teeth also may become extremely sensitive to
hot and cold stimuli.
• Osteoradionecrosis: Necrosis (death) of bone after
radiation treatment.
Copyright © 2005 by Elsevier Inc. All rights reserved.
Fig. 17-28 A and B, Radiation mucositis. C, Postradiation xerostomia.
(From Ibsen OC, Phelan JA: Oral pathology for the dental hygienist, ed 4, St. Louis, 2004, Saunders.)
Copyright © 2005 by Elsevier Inc. All rights reserved.
Acquired Immunodeficiency Syndrome
(AIDS)
• Oral lesions are prominent features of AIDS and
human immunodeficiency virus (HIV) infection.
• Oral lesions develop because of the breakdown of
the immune system that occurs when the T-helper
cells become depleted because of the disease.
Copyright © 2005 by Elsevier Inc. All rights reserved.
• Because the patient’s immune system is severely
damaged, death is usually caused by an
opportunistic infection.
• An opportunistic infection is one that normally would
be controlled by the immune system but that cannot
be controlled because of the HIV/AIDS, the immune
system is not functioning properly.
• It is important to remember that some of the lesions
that look like HIV- and AIDS-related infection may
also be caused by other disorders.
Copyright © 2005 by Elsevier Inc. All rights reserved.
HIV-Associated Gingivitis
• There is often a bright red line along the border of
the free gingival margin.
• Also known as atypical gingivitis (ATYP).
• In some cases, there may be progression of the
bright red line from the free gingival margin over
the attached gingival and alveolar mucosa.
Copyright © 2005 by Elsevier Inc. All rights reserved.
HIV-Associated Periodontitis
• HIV-associated periodontitis resembles acute
necrotizing ulcerative gingivitis superimposed
on rapidly progressive periodontitis.
• Other symptoms include:
– Interproximal necrosis and cratering
– Marked swelling
– Intense erythema over the free and attached gingiva
– Intense pain
– Spontaneous bleeding and bad breath
Copyright © 2005 by Elsevier Inc. All rights reserved.
Fig. 17-29 A, typical periodontal disease
in a patient with HIV infection
(From Ibsen OC, Phelan JA: Oral pathology for the dental hygienist, ed 4, St. Louis, 2004, Saunders.)
Copyright © 2005 by Elsevier Inc. All rights reserved.
HIV Cervical Lymphadenopathy
• Enlargement of the cervical (neck) nodes
• Lymphadenopathy is frequently seen in
association with AIDS.
Copyright © 2005 by Elsevier Inc. All rights reserved.
Fig. 17-30 HIV cervical lymphadenopathy
(From Ibsen OC, Phelan JA: Oral pathology for the dental hygienist, ed 4, St. Louis, 2004, Saunders.)
Copyright © 2005 by Elsevier Inc. All rights reserved.
HIV Lymphoma
• HIV lymphoma is the general term used to describe
malignant disorders of the lymphoid tissue.
• In the immunocompromised individual, it may occur
as a solitary lump or nodule, a swelling, or a
nonhealing ulcer that occurs anywhere in the oral
cavity.
• The swelling may be ulcerated or may be covered
with intact, normal-appearing mucosa.
• Usually painful, the lesion grows rapidly in size and
may be the first evidence of lymphoma.
Copyright © 2005 by Elsevier Inc. All rights reserved.
Fig. 17-32 HIV lymphoma
(From Ibsen OC, Phelan JA: Oral pathology for the dental hygienist, ed 4, St. Louis, 2004, Saunders.)
Copyright © 2005 by Elsevier Inc. All rights reserved.
Hairy Leukoplakia
• Hairy leukoplakia can be an important early
manifestation of AIDS status.
• It is a filamentous white plaque usually found
unilaterally or bilaterally on the lateral borders
(sides) on the anterior portion of the tongue.
• It may spread to cover the entire dorsal surface of
the tongue. It can also appear on the buccal mucosa,
where it generally has a flat appearance.
Copyright © 2005 by Elsevier Inc. All rights reserved.
Fig. 17-33 Hairy leukoplakia
(From Ibsen OC, Phelan JA: Oral pathology for the dental hygienist, ed 4, St. Louis, 2004, Saunders.)
Copyright © 2005 by Elsevier Inc. All rights reserved.
Kaposi's Sarcoma
• Kaposi's sarcoma is one of the opportunistic
infections that occur in patients with HIV infection.
• Kaposi's sarcoma lesions may appear as multiple
bluish, blackish, or reddish blotches that are usually
flat in the early stages.
• At present, there is no effective treatment for
Kaposi’s sarcoma.
• Kaposi’s sarcoma is one of the intraoral lesions that
are used to diagnose AIDS.
Copyright © 2005 by Elsevier Inc. All rights reserved.
Fig. 17-34 Kaposi’s sarcoma in a patient
with AIDS. A, Skin. B, Gingivae.
(From Ibsen OC, Phelan JA: Oral pathology for the dental hygienist, ed 4, St. Louis, 2004, Saunders.)
Copyright © 2005 by Elsevier Inc. All rights reserved.
Herpes Simplex
• Herpes simplex lesions usually occur on the lip.
• In immunocompromised patients, the lesions may
occur throughout the mouth.
• An ulcer caused by the herpes virus that persists
for longer than 1 month could be an indicator of
AIDS.
• Patients that do not have HIV or AIDs may also
suffer from herpes.
Copyright © 2005 by Elsevier Inc. All rights reserved.
Fig. 17-35 Herpes simplex on the hard palate
of a patient with HIV infection
(From Ibsen OC, Phelan JA: Oral pathology for the dental hygienist, ed 4, St. Louis, 2004, Saunders.)
Copyright © 2005 by Elsevier Inc. All rights reserved.
Human Papillomavirus
• Human papillomavirus appears most commonly
in immunocompromised individuals.
• Diagnosis is made based on history, clinical
appearance, and biopsy.
• They are a common finding in patients with early
HIV infection.
• These warts appear spiky, and some have a raised,
cauliflower-like appearance.
Copyright © 2005 by Elsevier Inc. All rights reserved.
Fig. 17-36 Human papillomavirus on the lip of a patient with AIDS
(From Ibsen OC, Phelan JA: Oral pathology for the dental hygienist, ed 4, St. Louis, 2004, Saunders.)
Copyright © 2005 by Elsevier Inc. All rights reserved.
Developmental Disorders
Can result when there is a disturbance of the cells
during the period when the cells divide.
The result is usually a deformity of part of the body.
Copyright © 2005 by Elsevier Inc. All rights reserved.
Types of Developmental Disorders
• Inherited disorders: Different from developmental
disorders because they are caused by an abnormal gene.
• A congenital disorder: One that is present at birth. It can
be either inherited or developmental; however, the exact
cause of most congenital abnormalities is unknown.
• Genetic factors: Malformations often due to genetic
factors such as chromosome abnormalities.
• Environmental factors: Called teratogens and can include
infections, drugs, and exposure to radiation.
Copyright © 2005 by Elsevier Inc. All rights reserved.
Exostoses
• Exostosis is a benign bony growth projecting
outward from the surface of a bone.
• An exostosis also may be referred to as a torus.
(A torus is a bulging projection. The plural is tori.)
Copyright © 2005 by Elsevier Inc. All rights reserved.
Fig. 17-38 Torus palatinus
(From Ibsen OC, Phelan JA: Oral pathology for the dental hygienist, ed 4, St. Louis, 2004, Saunders.)
Copyright © 2005 by Elsevier Inc. All rights reserved.
Fig. 17-39 Torus mandibularis
(From Ibsen OC, Phelan JA: Oral pathology for the dental hygienist, ed 4, St. Louis, 2004, Saunders.)
Copyright © 2005 by Elsevier Inc. All rights reserved.
Disturbances in the
Development of the Jaw, Lips,
Palate, and Tongue
Copyright © 2005 by Elsevier Inc. All rights reserved.
Types of Developmental Disturbances
of the Jaw, Lips, Palate, and Tongue
• Cleft lip: Results when the maxillary and medial nasal
processes fail to fuse.
• Cleft palate: Results when the palatal shelves fail to
fuse with the primary palate.
• Cleft uvula: The mildest form of cleft palate. Cleft
palate, with or without cleft lip, occurs once in 2500
live births.
• Ankyloglossia: Often called “tongue-tied,” results in
a short lingual frenum that extends to the apex of the
tongue.
Copyright © 2005 by Elsevier Inc. All rights reserved.
Fig. 17-40 A newborn with bilateral complete cleft lip and palate.
Note severe angulation of the premaxillary segment.
(From Kaban LB, Troulis M: Pediatric oral and maxillofacial surgery, St. Louis, 2004, Saunders.)
Copyright © 2005 by Elsevier Inc. All rights reserved.
Fig. 17-41 Ankyloglossia
(From Ibsen OC, Phelan JA: Oral pathology for the dental hygienist, ed 4, St. Louis, 2004, Saunders.)
Copyright © 2005 by Elsevier Inc. All rights reserved.
Disturbances in
Tooth Development and Eruption
Copyright © 2005 by Elsevier Inc. All rights reserved.
Disturbances in Tooth Development
• Ameloblastoma is a tumor composed of remnants
of the dental lamina.
• Anodontia is the congenital absence of teeth.
• Supernumerary teeth are teeth in excess of the 32
normal permanent teeth.
• Macrodontia is abnormally large teeth.
• Microdontia is abnormally small teeth.
• Dens in dente (tooth within a tooth) results in the
formation of a small tooth-like mass of enamel and
dentin within the pulp.
Copyright © 2005 by Elsevier Inc. All rights reserved.
Fig. 17-42 Partial anodontia
(From Ibsen OC, Phelan JA: Oral pathology for the dental hygienist, ed 3, Philadelphia, 2000, Saunders.)
Copyright © 2005 by Elsevier Inc. All rights reserved.
Fig. 17-43 Radiograph showing two supernumerary teeth
in region of the permanent premolars
(From Ibsen OC, Phelan JA: Oral pathology for the dental hygienist, ed 4, St. Louis, 2004, Saunders.)
Copyright © 2005 by Elsevier Inc. All rights reserved.
Disturbances in Enamel Formation
• Amelogenesis imperfecta is a hereditary abnormality
in which there are hypoplasia-type defects in the
enamel formation.
• Hypocalcification is the incomplete calcification or
hardening of the enamel.
• Hereditary enamel hypoplasia is a type of
amelogenesis imperfecta that is characterized by
teeth with crowns that are hard and glossy, yellow,
and cone shaped or cylindrical.
Copyright © 2005 by Elsevier Inc. All rights reserved.
Fig. 17-47 Note loss of enamel in these teeth in a patient
with hypocalcified amelogenesis imperfecta.
(From Ibsen OC, Phelan JA: Oral pathology for the dental hygienist, ed 4, St. Louis, 2004, Saunders.)
Copyright © 2005 by Elsevier Inc. All rights reserved.
Abnormal Eruption of the Teeth
• Premature eruption is natal teeth present at birth.
• Neonatal teeth are those that erupt within the first
30 days of life.
• Ankylosis is deciduous teeth in which bone has
fused to cementum and dentin, preventing
exfoliation.
• Impaction occurs when any tooth remains unerupted
in the jaws beyond the time at which it should
normally erupt.
Copyright © 2005 by Elsevier Inc. All rights reserved.
Fig. 17-48 A radiograph of ankylosis of a deciduous molar
(Courtesy Dr. Margot Van Dis. From Ibsen OC, Phelan JA: Oral pathology for the dental hygienist, ed 4, St. Louis, 2004, Saunders.)
Copyright © 2005 by Elsevier Inc. All rights reserved.
Fig. 17-49 Impactions in mixed dentition
visible on a dental radiograph
Copyright © 2005 by Elsevier Inc. All rights reserved.
Additional Disturbances in
Tooth Development and Eruption
• Variation in form includes extra, missing, or fused
cusps or anomalies of roots; however, the most
common variations are peg-shaped teeth.
• Hutchinson's incisors are a variety of peg-shaped
teeth, usually associated with maternal syphilis.
• Fusion is the joining together of the dentin and
enamel of two or more separate developing teeth.
• Gemination is an attempt by the tooth bud to divide.
When this attempt is not successful, an incisal notch
indicates it.
Copyright © 2005 by Elsevier Inc. All rights reserved.
Miscellaneous Disorders
• Abrasion is the abnormal wearing away of tooth
structure that is caused by a repetitive mechanical
habit such as improper toothbrushing.
• Attrition is the normal wearing away of tooth
structure during mastication (chewing).
• Bruxism is an oral habit consisting of involuntary
gnashing, grinding, and clenching of the teeth in
movements other than chewing. It is usually
performed during sleep and is commonly associated
with stress or tension.
Copyright © 2005 by Elsevier Inc. All rights reserved.
Fig. 17-50 Abrasion at the cervical area of
mandibular premolars caused by toothbrushing.
(From Ibsen OC, Phelan JA: Oral pathology for the dental hygienist, ed 4, St. Louis, 2004, Saunders.)
Copyright © 2005 by Elsevier Inc. All rights reserved.
Fig. 17-51 A and B, Attrition of adult dentition
(From Ibsen OC, Phelan JA: Oral pathology for the dental hygienist, ed 4, St. Louis, 2004, Saunders.)
Copyright © 2005 by Elsevier Inc. All rights reserved.
Fig. 17-52 Bruxism caused attrition of the mandibular anterior teeth
(From Ibsen OC, Phelan JA: Oral pathology for the dental hygienist, ed 4, St. Louis, 2004, Saunders.)
Copyright © 2005 by Elsevier Inc. All rights reserved.
Miscellaneous Disorders-cont’d
• Bulimia is an eating disorder characterized by
food binges and followed by self-induced
vomiting.
• The dental professional is often the first health
care professional to identify a patient with
bulimia.
Copyright © 2005 by Elsevier Inc. All rights reserved.
Fig. 17-53 A and B, Erosion caused by bulimia
(From Ibsen OC, Phelan JA: Oral pathology for the dental hygienist, ed 4, St. Louis, 2004, Saunders.)
A B
Copyright © 2005 by Elsevier Inc. All rights reserved.
S-ar putea să vă placă și
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeDe la EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeEvaluare: 4 din 5 stele4/5 (5794)
- Cancer Prediction and Prognosis Using Machine Learning TechniquesDocument5 paginiCancer Prediction and Prognosis Using Machine Learning TechniquesInternational Journal of Innovative Science and Research TechnologyÎncă nu există evaluări
- The Little Book of Hygge: Danish Secrets to Happy LivingDe la EverandThe Little Book of Hygge: Danish Secrets to Happy LivingEvaluare: 3.5 din 5 stele3.5/5 (400)
- Gynecology 1.1 - History-Taking, Physical Examination, and Office GynecologyDocument9 paginiGynecology 1.1 - History-Taking, Physical Examination, and Office GynecologyZaza100% (2)
- Shoe Dog: A Memoir by the Creator of NikeDe la EverandShoe Dog: A Memoir by the Creator of NikeEvaluare: 4.5 din 5 stele4.5/5 (537)
- Cell Division LabDocument5 paginiCell Division Labjenna727Încă nu există evaluări
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceDe la EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceEvaluare: 4 din 5 stele4/5 (895)
- Hartmann Procedure - Google SearchDocument1 paginăHartmann Procedure - Google SearchGrizzel CortesÎncă nu există evaluări
- The Yellow House: A Memoir (2019 National Book Award Winner)De la EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Evaluare: 4 din 5 stele4/5 (98)
- DohDocument8 paginiDohJai MacanasÎncă nu există evaluări
- The Emperor of All Maladies: A Biography of CancerDe la EverandThe Emperor of All Maladies: A Biography of CancerEvaluare: 4.5 din 5 stele4.5/5 (271)
- Xerostomia - Understanding The Diagnosis and The Treatment of Dry MouthDocument5 paginiXerostomia - Understanding The Diagnosis and The Treatment of Dry MouthferifhransÎncă nu există evaluări
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryDe la EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryEvaluare: 3.5 din 5 stele3.5/5 (231)
- MSDS Crude OilDocument6 paginiMSDS Crude OilFabio IkaczykÎncă nu există evaluări
- Never Split the Difference: Negotiating As If Your Life Depended On ItDe la EverandNever Split the Difference: Negotiating As If Your Life Depended On ItEvaluare: 4.5 din 5 stele4.5/5 (838)
- APE QuestionsDocument6 paginiAPE QuestionsJahg WongÎncă nu există evaluări
- Grit: The Power of Passion and PerseveranceDe la EverandGrit: The Power of Passion and PerseveranceEvaluare: 4 din 5 stele4/5 (588)
- Clomid - (Clomiphene CitrateDocument13 paginiClomid - (Clomiphene Citrateboron32Încă nu există evaluări
- On Fire: The (Burning) Case for a Green New DealDe la EverandOn Fire: The (Burning) Case for a Green New DealEvaluare: 4 din 5 stele4/5 (73)
- Assessment of Food Intakes For Women Adopting The High Protein Dukan DietDocument6 paginiAssessment of Food Intakes For Women Adopting The High Protein Dukan DietDevi Arine KusumawardaniÎncă nu există evaluări
- Interpreting Chest FilmsDocument122 paginiInterpreting Chest Filmsgeorgen1Încă nu există evaluări
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureDe la EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureEvaluare: 4.5 din 5 stele4.5/5 (474)
- Malabsorption Syndrome: Dr. Md. Golam Kibria Khan Associate Professor of Medicine Medicine Unit - Iv MMCHDocument20 paginiMalabsorption Syndrome: Dr. Md. Golam Kibria Khan Associate Professor of Medicine Medicine Unit - Iv MMCHThunder BoltÎncă nu există evaluări
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaDe la EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaEvaluare: 4.5 din 5 stele4.5/5 (266)
- Medical Surgical Nursing TionkoDocument40 paginiMedical Surgical Nursing TionkojeshemaÎncă nu există evaluări
- The Unwinding: An Inner History of the New AmericaDe la EverandThe Unwinding: An Inner History of the New AmericaEvaluare: 4 din 5 stele4/5 (45)
- Approach To Patients EULARDocument35 paginiApproach To Patients EULARstuckinbedÎncă nu există evaluări
- PI MaltoferDocument15 paginiPI MaltoferrazhossenÎncă nu există evaluări
- Team of Rivals: The Political Genius of Abraham LincolnDe la EverandTeam of Rivals: The Political Genius of Abraham LincolnEvaluare: 4.5 din 5 stele4.5/5 (234)
- Lesson: Dr. Leon Hammer, M.DDocument14 paginiLesson: Dr. Leon Hammer, M.DRocío JMÎncă nu există evaluări
- Abdominal ExaminationDocument16 paginiAbdominal ExaminationLana IbrahimÎncă nu există evaluări
- CML Learning Programme For Nurses & Other Allied Health Care ProfessionalsDocument75 paginiCML Learning Programme For Nurses & Other Allied Health Care ProfessionalsSuci Prima AnggrainiÎncă nu există evaluări
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyDe la EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyEvaluare: 3.5 din 5 stele3.5/5 (2259)
- Portfolio Clinical Case Study 2Document29 paginiPortfolio Clinical Case Study 2api-277136509Încă nu există evaluări
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreDe la EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreEvaluare: 4 din 5 stele4/5 (1090)
- Medical PediatricDocument358 paginiMedical PediatricAishah Alsaud100% (10)
- (Urinary System, Digestive System and Nervous System) : My Lost HopesDocument3 pagini(Urinary System, Digestive System and Nervous System) : My Lost HopesCesar Dave PresentacionÎncă nu există evaluări
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersDe la EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersEvaluare: 4.5 din 5 stele4.5/5 (344)
- Pharmacology of Testosterone: Made By: Miangul Ali GoharDocument21 paginiPharmacology of Testosterone: Made By: Miangul Ali GoharAli GoharÎncă nu există evaluări
- Underground Clinical Vignettes BiochemistryDocument128 paginiUnderground Clinical Vignettes Biochemistrymartha2112Încă nu există evaluări
- 237 Goljan Rapid Review Images FlashcardsDocument34 pagini237 Goljan Rapid Review Images FlashcardsAhsan Tanvir100% (1)
- BPH PSPD 2012Document43 paginiBPH PSPD 2012Nor AinaÎncă nu există evaluări
- Breast US - AAR 2004Document73 paginiBreast US - AAR 2004donÎncă nu există evaluări
- CCU AuditDocument75 paginiCCU AuditNica Reyes-Sindiong0% (1)
- DSM V - OcdDocument10 paginiDSM V - OcdNidhiÎncă nu există evaluări
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)De la EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Evaluare: 4.5 din 5 stele4.5/5 (121)
- 1358453842.3856hematology Question BankDocument182 pagini1358453842.3856hematology Question BankKay BristolÎncă nu există evaluări
- Gastric VolvulusDocument6 paginiGastric VolvulusIosif SzantoÎncă nu există evaluări
- Her Body and Other Parties: StoriesDe la EverandHer Body and Other Parties: StoriesEvaluare: 4 din 5 stele4/5 (821)