Documente Academic
Documente Profesional
Documente Cultură
Implantation
Încărcat de
Gian Paolo Sisona0 evaluări0% au considerat acest document util (0 voturi)
8 vizualizări43 paginiLearnings
Drepturi de autor
© © All Rights Reserved
Formate disponibile
PPTX, PDF, TXT sau citiți online pe Scribd
Partajați acest document
Partajați sau inserați document
Vi se pare util acest document?
Este necorespunzător acest conținut?
Raportați acest documentLearnings
Drepturi de autor:
© All Rights Reserved
Formate disponibile
Descărcați ca PPTX, PDF, TXT sau citiți online pe Scribd
0 evaluări0% au considerat acest document util (0 voturi)
8 vizualizări43 paginiImplantation
Încărcat de
Gian Paolo SisonaLearnings
Drepturi de autor:
© All Rights Reserved
Formate disponibile
Descărcați ca PPTX, PDF, TXT sau citiți online pe Scribd
Sunteți pe pagina 1din 43
• spontaneous, cyclical ovulation at 25- to 35-day intervals continues
during almost 40 years between menarche and menopause
• 400 opportunities for pregnancy, which may occur with intercourse
on any of 1200 days—the day of ovulation and its two preceding days.
• placenta mediates a unique fetal–maternal communication system,
which creates a hormonal environment that initially maintains
pregnancy and eventually initiates events leading to parturition
• Predictable, regular, cyclical, and spontaneous ovulatory menstrual
cycles are regulated by complex interactions of the hypothalamic-
pituitary axis, ovaries, and genital tract.
• The average cycle duration is approximately 28 days, with a range of
25 to 32 days.
The Ovarian Cycle
• Follicular or Preovulatory Ovarian Phase
• Ovulation
• Luteal or Postovulatory Ovarian Phase
Follicular or Preovulatory Phase
• Ovary: 2 million oocytes (birth) and approximately 400,000 follicles
(puberty)
• Remaining follicles: depleted at a rate of approximately 1000 follicles/month
until age 35
• Only 400 follicles are normally released during female reproductive
life.
• >99.9% of follicles undergo atresia via apoptosis
Ovulation
• gonadotropin surge: 34 to 36 hours before ovum release from the
follicle
• from increasing estrogen secretion by preovulatory follicles
• relatively precise predictor of ovulation
• LH secretion peaks 10 to 12 hours before ovulation
• stimulates resumption of meiosis in the ovum and release of the first polar
body.
Luteal or Postovulatory Ovarian Phase
• luteinization: corpus luteum develops from the dominant or Graafian
follicle remains
• LH: corpus luteum maintenance
• The human corpus luteum is a transient endocrine organ that, in the
absence of pregnancy, will rapidly regress 9 to 11 days after ovulation
via apoptotic cell death.
• from decreased levels of circulating LH in the late luteal phase and decreased
LH sensitivity of luteal cells
Estrogen
• 17β-estradiol: is secreted by granulosa cells of the dominant follicle
and luteinized granulosa cells of the corpus luteum
• two classic nuclear hormone receptors: estrogen receptor α (ERα) and
β (ERβ)
Progesterone
• progesterone receptor type A (PR-A) and B (PR-B)
• enters cells by diffusion and in responsive tissues becomes associated
with progesterone receptors
The Endometrial Cycle
• Proliferative or Preovulatory Endometrial Phase
• Secretory or Postovulatory Endometrial Phase
• Menstruation
Proliferative Phase
Early Secretory Phase
Secretory Phase
• Estradiol action is decreased.
• rising progesterone levels >> glandular cell mitosis ceases with secretory
activity
• glandular expression of the type 2 isoform of 17β-hydroxysteroid
dehydrogenase >> estradiol to estrone
Late Secretory Phase
Menstruation
• Leukocyte infiltration: key to both endometrial extracellular matrix
breakdown and repair of the functionalis layer.
• “inflammatory tightrope”: ability of macrophages to assume
phenotypes that vary from proinflammatory and phagocytic to
immunosuppressive and reparative.
• Invading leukocytes secrete enzymes of the matrix metalloprotease
(MMP) family. These add to the proteases already produced by
endometrial stromal cells and effectively initiate matrix degradation.
• As tissue shedding is completed, microenvironment-regulated
changes in macrophage phenotype promote repair and resolution.
Menstruation
Anatomical Events
• endometrial regression >> severe spiral artery coiling >> inc resistance
to blood flow >> endometrial hypoxia
• Resultant stasis: primary cause of endometrial ischemia and tissue
degeneration.
• Vasoconstriction precedes menstruation and is the most striking and
constant event observed in the cycle.
• Intense spiral artery vasoconstriction: limits menstrual blood loss.
Prostaglandins
• Progesterone withdrawal >> inc expression of COX-2 (prostaglandin
synthase 2) >> prostaglandin synthesis
• Withdrawal >> dec expression of 15-hydroxyprostaglandin
dehydrogenase (PGDH) >> increased prostaglandin production by
endometrial stromal cells and increased prostaglandin receptor
density on blood vessels and surrounding cells.
• Dysmenorrhea: mediated by PGF 2α -induced spiral artery
vasoconstriction that causes the uppermost endometrial zones to
become hypoxic.
Menstrual blood
• Arterial
• rupture of a spiral arteriole >> hematoma >> distention and eventual
rupture of superficial endometrium >> fissures develop in the
adjacent functionalis layer >> sloughing off of blood and tissue
fragments >> endometrial bleeding
• Hemorrhage stops with arteriolar constriction and changes
accompanying partial tissue necrosis also serve to seal vessel tips.
Endometrium
• The endometrial surface is restored by growth of flanges, or collars,
that form the everted free ends of the endometrial glands.
• These flanges increase in diameter very rapidly, and epithelial continuity is
reestablished by fusion of the edges of these sheets of migrating cells.
Interval between menses
• The modal interval of menstruation is considered to be 28 days
Decidua
• specialized, highly modified endometrium of pregnancy.
• essential for hemochorial placentation
• Decidualization: transformation of secretory endometrium to decidua
• is dependent on estrogen and progesterone and factors secreted by the
implanting blastocyst.
Decidua
• early pregnancy: the decidua begins to thicken (depth of 5 to 10 mm).
• With magnification, furrows and numerous small openings, representing the
mouths of uterine glands, can be detected.
• late pregnancy: the decidua becomes thinner.
• pressure exerted by the expanding uterine contents
Decidua
• 3 layers of decidua parietalis and basalis:
• zona compacta: surface or compact zone
• zona spongiosa: a middle portion or spongy zone, with remnants of
glands and numerous small blood vessels
• zona basalis: basal zone
• remains after delivery and gives rise to new endometrium
• zona functionalis= compacta + spongiosa
Decidual Reaction
• completed only with blastocyst implantation
• Predecidual changes: during the midluteal phase in endometrial stromal
cells adjacent to the spiral arteries and arterioles. Thereafter, they spread
in waves throughout the uterine endometrium and then from the
implantation site.
• endometrial stromal cells: enlarge to form polygonal or round decidual
cells
• Nuclei: round and vesicular
• Cytoplasm: clear, slightly basophilic, and surrounded by a translucent
membrane. Each mature decidual cell becomes surrounded by a
pericellular membrane.
Decidual Reaction
• endometrial stromal cells: enlarge to form polygonal or round
decidual cells
• Nuclei: round and vesicular
• Cytoplasm: clear, slightly basophilic, and surrounded by a translucent
membrane
• pericellular membrane: surrounds each mature decidual cell
Decidual Blood Supply
• BS to the decidua capsularis is lost as the embryo-fetus grows.
• BS to the decidua parietalis through spiral arteries persists and retain
a smooth-muscle wall and endothelium >> responsive to vasoactive
agents.
Decidual Blood Supply
• The spiral arterial system supplying the decidua basalis are invaded by
cytotrophoblasts. The vessel walls in the basalis are destroyed. Only a
shell without smooth muscle or endothelial cells remains >> not
responsive to vasoactive agents.
• fetal chorionic vessels (transport blood between the placenta and the
fetus): contain smooth muscle >> respond to vasoactive agents.
Decidual Histology
• Early: zona spongiosa consists of large distended glands, often
exhibiting marked hyperplasia and separated by minimal stroma.
• glands are lined by typical cylindrical uterine epithelium with abundant
secretory activity that contributes to blastocyst nourishment
• Late: epithelium gradually becomes cuboidal or even flattened >>
degenerates and sloughs to a greater extent into the gland lumens >>
glandular elements largely disappear
Decidual Histology
• The decidua basalis contributes to formation of the placental basal
plate.
• differs histologically from the decidua parietalis
• spongy zone of the decidua basalis: mainly of arteries and widely dilated
veins, and by term, glands have virtually disappeared
• decidua basalis is invaded by many interstitial trophoblast cells and
trophoblastic giant cells
Decidual Histology
• Nitabuch layer: is a zone of fibrinoid degeneration in which invading
trophoblasts meet the decidua basalis.
• Rohr stria: more superficial, but inconsistent, deposition of fibrin at
the bottom of the intervillous space and surrounding the anchoring
villi.
• Early: a striking abundance of large, granular lymphocytes termed
decidual natural killer (NK) cells
• important role in trophoblast invasion and vasculogenesis.
Decidual Prolactin
• prolactin levels in amnionic fluid are extraordinarily high and may
reach 10,000 ng/ mL at 20 to 24 weeks’ gestation
• fetal serum levels of 350 ng/mL and maternal serum levels of 150 to
200 ng/mL
• paracrine function between maternal and fetal tissues
Decidual Prolactin
• may serve in transmembrane solute and water transport and in
amnionic fluid volume maintenance.
• may act in regulating immunological functions during pregnancy.
• may play a role in angiogenesis regulation during implantation.
Fertilization and Implantation
Zygote
• After fertilization
• Diploid cell with 46 Chromosomes
Morula
• a solid mulberry-like ball of cells
• morula enters the uterine cavity
about 3 days after fertilization.
Blastocyst
• 4 to 5 days after fertilization
• measures approximately 0.155 mm in diameter
Blastocyst Implantation
• 6 or 7 days after fertilization
• 3 phases:
• Apposition
• Adhesion – integrin
• Invasion
S-ar putea să vă placă și
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryDe la EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryEvaluare: 3.5 din 5 stele3.5/5 (231)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)De la EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Evaluare: 4.5 din 5 stele4.5/5 (119)
- Never Split the Difference: Negotiating As If Your Life Depended On ItDe la EverandNever Split the Difference: Negotiating As If Your Life Depended On ItEvaluare: 4.5 din 5 stele4.5/5 (838)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaDe la EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaEvaluare: 4.5 din 5 stele4.5/5 (265)
- The Little Book of Hygge: Danish Secrets to Happy LivingDe la EverandThe Little Book of Hygge: Danish Secrets to Happy LivingEvaluare: 3.5 din 5 stele3.5/5 (399)
- Grit: The Power of Passion and PerseveranceDe la EverandGrit: The Power of Passion and PerseveranceEvaluare: 4 din 5 stele4/5 (587)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyDe la EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyEvaluare: 3.5 din 5 stele3.5/5 (2219)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeDe la EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeEvaluare: 4 din 5 stele4/5 (5794)
- Team of Rivals: The Political Genius of Abraham LincolnDe la EverandTeam of Rivals: The Political Genius of Abraham LincolnEvaluare: 4.5 din 5 stele4.5/5 (234)
- Shoe Dog: A Memoir by the Creator of NikeDe la EverandShoe Dog: A Memoir by the Creator of NikeEvaluare: 4.5 din 5 stele4.5/5 (537)
- The Emperor of All Maladies: A Biography of CancerDe la EverandThe Emperor of All Maladies: A Biography of CancerEvaluare: 4.5 din 5 stele4.5/5 (271)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreDe la EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreEvaluare: 4 din 5 stele4/5 (1090)
- Her Body and Other Parties: StoriesDe la EverandHer Body and Other Parties: StoriesEvaluare: 4 din 5 stele4/5 (821)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersDe la EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersEvaluare: 4.5 din 5 stele4.5/5 (344)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceDe la EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceEvaluare: 4 din 5 stele4/5 (890)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureDe la EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureEvaluare: 4.5 din 5 stele4.5/5 (474)
- The Unwinding: An Inner History of the New AmericaDe la EverandThe Unwinding: An Inner History of the New AmericaEvaluare: 4 din 5 stele4/5 (45)
- The Yellow House: A Memoir (2019 National Book Award Winner)De la EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Evaluare: 4 din 5 stele4/5 (98)
- On Fire: The (Burning) Case for a Green New DealDe la EverandOn Fire: The (Burning) Case for a Green New DealEvaluare: 4 din 5 stele4/5 (73)
- Abnormal Uterine BleedingDocument23 paginiAbnormal Uterine BleedingTakeru Ferry100% (1)
- Pharmacology of Drugs Acting On Uterus - MBBSDocument23 paginiPharmacology of Drugs Acting On Uterus - MBBSDr.U.P.Rathnakar.MD.DIH.PGDHM100% (5)
- Final Exam Saudi Board 2009Document38 paginiFinal Exam Saudi Board 2009Aloah122346Încă nu există evaluări
- Placenta Previa Case StudyDocument59 paginiPlacenta Previa Case StudySiergs Smith GervacioÎncă nu există evaluări
- Leptospirosis CPG 2010 PDFDocument66 paginiLeptospirosis CPG 2010 PDFRogelio Junior RiveraÎncă nu există evaluări
- gr080005 PDFDocument3 paginigr080005 PDFGian Paolo SisonaÎncă nu există evaluări
- Anae 12034Document8 paginiAnae 12034Gian Paolo SisonaÎncă nu există evaluări
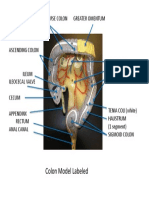
- Colon Model LabeledDocument1 paginăColon Model LabeledGian Paolo SisonaÎncă nu există evaluări
- Test Normal Values Patient Values Interpreta Tion of Results Availabilit y CostDocument1 paginăTest Normal Values Patient Values Interpreta Tion of Results Availabilit y CostGian Paolo SisonaÎncă nu există evaluări
- KyrlllllllllllllDocument1 paginăKyrlllllllllllllGian Paolo SisonaÎncă nu există evaluări
- March 18 2013: MU DN CF PW BB GC PB HON LOL KOS Cabal Shaiya MerDocument1 paginăMarch 18 2013: MU DN CF PW BB GC PB HON LOL KOS Cabal Shaiya MerGian Paolo SisonaÎncă nu există evaluări
- Pregnancy Assessment Health History ROSDocument34 paginiPregnancy Assessment Health History ROSteuuuuÎncă nu există evaluări
- Ekwo 1993Document10 paginiEkwo 1993Nurul ImaniarÎncă nu există evaluări
- Case Presentation OB - GYNDocument14 paginiCase Presentation OB - GYNRaidah Ayesha RazackÎncă nu există evaluări
- Ectopic Pregnancy: Deomicah D. SolanoDocument42 paginiEctopic Pregnancy: Deomicah D. SolanoJann ericka JaoÎncă nu există evaluări
- Superior Hypogastric Plexus Anatomy QuizDocument4 paginiSuperior Hypogastric Plexus Anatomy QuizMaryneth EvangelistaÎncă nu există evaluări
- InfertilityDocument5 paginiInfertilityRupert BautistaÎncă nu există evaluări
- M. Preterm and Postterm - NewDocument92 paginiM. Preterm and Postterm - NewTry Ariditya UtomoÎncă nu există evaluări
- Metformin Use in Women With Polycystic Ovary Syndrome: Neil P. JohnsonDocument6 paginiMetformin Use in Women With Polycystic Ovary Syndrome: Neil P. JohnsonanyÎncă nu există evaluări
- Ob Talking Points Efm:: W.I.N.KDocument4 paginiOb Talking Points Efm:: W.I.N.KRon ChurrascoÎncă nu există evaluări
- Gynaecology QuestionsDocument19 paginiGynaecology QuestionsShaik AmreenÎncă nu există evaluări
- O&G EMQsDocument10 paginiO&G EMQsV SugrimÎncă nu există evaluări
- Know About The Best Gynecologists in Delhi NCRDocument9 paginiKnow About The Best Gynecologists in Delhi NCRSimi AhujaÎncă nu există evaluări
- Case Reports in Women's Health: Tanja Baltus Maria Luisa MartinDocument2 paginiCase Reports in Women's Health: Tanja Baltus Maria Luisa MartinDavid LacosteÎncă nu există evaluări
- Jurnal Gentle BirthDocument5 paginiJurnal Gentle BirthIka KarimahÎncă nu există evaluări
- Cabbage Leaves Effective in Reducing Breast Milk DamsDocument6 paginiCabbage Leaves Effective in Reducing Breast Milk DamsAmeliarÎncă nu există evaluări
- Science 10 - Quiz 1 - Q3W1Document1 paginăScience 10 - Quiz 1 - Q3W1ChelleÎncă nu există evaluări
- Routine Episiotomy For Vaginal Birth: Should It Be Ignored?Document8 paginiRoutine Episiotomy For Vaginal Birth: Should It Be Ignored?IOSRjournalÎncă nu există evaluări
- Obesity and PregnancyDocument4 paginiObesity and PregnancyRL FlacamaÎncă nu există evaluări
- Accuracy of Tubal Patency Assessment in Diagnostic Hysteroscopy Compared With Laparoscopy in Infertile WomenDocument20 paginiAccuracy of Tubal Patency Assessment in Diagnostic Hysteroscopy Compared With Laparoscopy in Infertile Womenria.janitaÎncă nu există evaluări
- Operational - Guidelines For Breastfeeding MAA 2022Document36 paginiOperational - Guidelines For Breastfeeding MAA 2022mrs raamÎncă nu există evaluări
- 133 Ritgen - JMFNM - AquinoDocument9 pagini133 Ritgen - JMFNM - AquinoDavid A Tovar OÎncă nu există evaluări
- Curs EnglezaDocument257 paginiCurs EnglezaFlorina CarolÎncă nu există evaluări
- Endocervical Adenocarcinoma in Situ Presenting in Fundal Endometrial Polyp: The Mother of All Skip LesionsDocument4 paginiEndocervical Adenocarcinoma in Situ Presenting in Fundal Endometrial Polyp: The Mother of All Skip LesionsAnonymous YyLSRdÎncă nu există evaluări
- Oral Contraceptive InstructionsDocument2 paginiOral Contraceptive Instructionsmiracle jefferyÎncă nu există evaluări
- Partograph: A Graphical Record Of Labor Progress And ConditionsDocument49 paginiPartograph: A Graphical Record Of Labor Progress And Conditionsdr jai gurungÎncă nu există evaluări
- Body System: Reproductive - FemaleDocument2 paginiBody System: Reproductive - FemaleKakah MoÎncă nu există evaluări