Documente Academic
Documente Profesional
Documente Cultură
Diabetic Ketoacidosis (Dka)
Încărcat de
yazid100%(5)100% au considerat acest document util (5 voturi)
3K vizualizări16 paginiDKA is an ACUTE, MAJOR, LIFE-THREATENING complication of diabetes. Is consequence of absolute or relative insulin deficiency with increase in counter-regulatory hormones. Characterized by hyperglycemia, acidosis, and ketonuria.
Descriere originală:
Titlu original
diabetic ketoacidosis (dka)
Drepturi de autor
© Attribution Non-Commercial (BY-NC)
Formate disponibile
PPT, PDF, TXT sau citiți online pe Scribd
Partajați acest document
Partajați sau inserați document
Vi se pare util acest document?
Este necorespunzător acest conținut?
Raportați acest documentDKA is an ACUTE, MAJOR, LIFE-THREATENING complication of diabetes. Is consequence of absolute or relative insulin deficiency with increase in counter-regulatory hormones. Characterized by hyperglycemia, acidosis, and ketonuria.
Drepturi de autor:
Attribution Non-Commercial (BY-NC)
Formate disponibile
Descărcați ca PPT, PDF, TXT sau citiți online pe Scribd
100%(5)100% au considerat acest document util (5 voturi)
3K vizualizări16 paginiDiabetic Ketoacidosis (Dka)
Încărcat de
yazidDKA is an ACUTE, MAJOR, LIFE-THREATENING complication of diabetes. Is consequence of absolute or relative insulin deficiency with increase in counter-regulatory hormones. Characterized by hyperglycemia, acidosis, and ketonuria.
Drepturi de autor:
Attribution Non-Commercial (BY-NC)
Formate disponibile
Descărcați ca PPT, PDF, TXT sau citiți online pe Scribd
Sunteți pe pagina 1din 16
إعداد و تقدي طلب سنة سادسة
سهر العلي – معاذ عيّاد – يزيد جبيل
Objectives
Definition of DKA and its Pathophysiology
Causes and precipitating factors
Clinical features by history and physical
examination
Investigations for DKA (Diagnosis &
Monitoring)
Management
Complications
Prognosis.
Introduction
Diabetic ketoacidosis (DKA) is an ACUTE,
MAJOR, LIFE-THREATENING complication of
diabetes.
DKA is defined:
o Clinically as an acute state of severe
uncontrolled diabetes that requires emergency
treatment with insulin and intravenous fluids.
o Biochemically as an increase in the serum
concentration of ketones greater than 5 mEq/L,
a blood glucose level of greater than 250 mg/dL
(although it is usually much higher), blood pH of
less than 7.2, and a bicarbonate level of 18
mEq/L or less.
Pathophysiology
DKA is characterized by hyperglycemia, acidosis, and
ketonuria.
DKA is consequence of absolute or relative insulin
deficiency with increase in counter-regulatory
hormones .
↓Insulin and ↑counter-regulatory hormone→
1. Gluconeogenesis and glycogenolysis → Hyperglycemia .
2. Lipolysis → Free Fatty Acids → Ketogenesis →
Ketonemia and ketonuria→ ↓ pH and bicarbonate serum
levels→ Metabolic acidosis → Ketoacidosis.
Pathophysiology cont.
Hyperglycemia→ Glycosuria→ Osmotic diuresis→
dehydration and tissue hypoperfusion.
Hyperglycemia, osmotic diuresis, serum
hyperosmolarity, and metabolic acidosis→
concentration disturbance.
Osmotic diuresis→ Potassium Sodium loss in the urine.
High serum osmolarity→ Dilutional hyponatremia.
Causes and Precipitating
Factors
The most common Other precipitants
precipitants 2.CVA
3.Intracranial bleeding
2.Infections (30–50%): 4.Acute pulmonary embolism
pneumonia, urinary tract 5.Intestinal or mesenteric thrombosis
6.Intestinal obstruction
infections, sepsis,
7.Acute pancreatitis
gastroenteritis 8.Alcohol intoxication or abuse
3.Inadequate insulin treatment 9.Severe burns, hyperthermia or
hypothermia
(20–40%): includes 10.Endocrine disorders: Cushing's
noncompliance, insulin pump syndrome, thyrotoxicosis,
failure acromegaly
11.Total parenteral nutrition
4.Myocardial ischemia or 12.Drugs: β-blockers, diuretics,
infarction (3–6%): often corticosteroids, antipsychotics
Clinical Features
Symptoms: Signs:
2.Polydypsia. 2.Dehydration:
3.Polyuria. o Dry skin and mucous .
4.Hyperglycemia. o Orthostatic
5.Nausea, lethargy, hypotension.
anorexia, weakness. o Tachycardia.
6.Abdominal pain. o Reduced JVP.
7.Reduced motility of GI. o Reduced mental
8.Vomiting. function
3.Ketosis:
Diagnosis
Table -1 Diagnostic criteria for diabetic ketoacidosis and the
hyperosmolar hyperglycemic state
Mild DKA Moderate DKA Severe DKA
Plasma glucose (mg/dL) >250 >250 >250
Effective serum osmolality (mOsm/kg) Variable Variable Variable
Urine or serum ketones (NP reaction) Positive Positive Positive
Arterial pH 7.25–7.30 7.00–7.24 <7.00
Serum bicarbonate (mEq/L) 15–18 10–15 <10
Anion gap (mEq/L) >10 >12 >12
Typical mental status Alert Drowsy Stupor or coma
Investigations
Glucose level.
Serum Ketones.
Acid-base status: pH, Serum bicarbonate and
Anion gap.
Electrolytes: Na +K+ Cl - Mg +2
ECG
CBC, WBC.
Urinalysis.
Cardiac markers, Liver enzymes and Amylase.
Chest X-Ray.
Blood and urine culture.
Management
Confirm diagnosis and admit to hospital or
ICU.
Assess:
o Serum electrolytes, Acid-base status and Renal
function.
Replace fluids:
o 2–3 L of 0.9% saline over first 1–3 h (10–15
mL/kg per hour);
o subsequently, 0.45% saline at 150–300 mL/h;
o change to 5% glucose and 0.45% saline at 100–
Management cont.
Administer short acting insulin: IV (0.1
units/kg) or IM (0.3 units/kg), then 0.1
units/kg/hour by continuous IV infusion; increase
2- to 3-fold if no response by 2–4 h. If initial serum
K+ is < 3.3 mmol/L ,do not administer insulin until
the potassium is corrected to > 3.3 mmol/L.
Assess patient: What precipitated the episode
(noncompliance, infection, trauma, infarction,
cocaine)? Initiate appropriate workup for
precipitating event (cultures, CXR, ECG).
Measure capillary glucose every 1–2 h; measure
electrolytes (especially K+, bicarbonate,
Management cont.
Monitor vital signs, mental status, fluid intake
and output every 1–4 h.
Replace K+: 10 mEq/h when plasma K+ < 5.5
mEq/L, ECG normal, urine flow and normal
creatinine documented; administer 40–80 mEq/h
when plasma K+ < 3.5 mEq/L or if bicarbonate is
given.
Continue above until patient is stable,
glucose goal is 150–250 mg/dL, and
acidosis is resolved. Insulin infusion may be
decreased to 0.05–0.1 units/kg per hour.
Administer intermediate or long-acting insulin as
soon as patient is eating. Allow for overlap in
Complications
Cerebral edema
Cardiac dysrhythmia
Pulmonary edema
Nonspecific myocardial injury may occur in
severe DKA.
Microvascular changes consistent with diabetic
retinopathy.
Prognosis
Excellent: especially in younger patients if
intercurrent infections are absent.
The worst prognosis: is usually observed in
patients who are older with severe
intercurrent illnesses, eg, myocardial
infarction, sepsis, or pneumonia, especially
when they are treated outside an ICU.
signs of poor prognosis: deep coma at the
time of diagnosis, hypothermia, and oliguria.
References
Cecil Medicine, 23rd Ed
Harrison's Principles of Internal Medicine, 17th
Edition, 2008
eMedicine.com Specialties > Endocrinology >
Diabetes Mellitus
Thank You
Any Questions ?
S-ar putea să vă placă și
- Myocardial InfarctionDocument18 paginiMyocardial Infarctionporing500Încă nu există evaluări
- Pathology+101 Complete)Document147 paginiPathology+101 Complete)Goh Kah Yong100% (2)
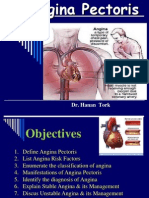
- Angina PectorisDocument38 paginiAngina Pectorisekhafagy100% (1)
- Complications of Diabetes Mellitus-UpdateDocument48 paginiComplications of Diabetes Mellitus-UpdateAnditha Namira RS100% (1)
- Chronic Renal FailureDocument46 paginiChronic Renal Failurestepharry08100% (1)
- Liver Cirrhosis: Review HepatologyDocument71 paginiLiver Cirrhosis: Review HepatologyAstri Arri FebriantiÎncă nu există evaluări
- Diabetic Ketoacidosis (DKA) VS. Hyperosmolar Hyperglycemic Syndrome (HHS)Document5 paginiDiabetic Ketoacidosis (DKA) VS. Hyperosmolar Hyperglycemic Syndrome (HHS)MrRightÎncă nu există evaluări
- Pulmonary Edema: (Acute Heart Failure)Document7 paginiPulmonary Edema: (Acute Heart Failure)james garcia100% (5)
- Angina PectorisDocument11 paginiAngina Pectorisjialin80% (5)
- Acute Kidney FailureDocument8 paginiAcute Kidney FailureRaidis PangilinanÎncă nu există evaluări
- ARDS With PathophysiologyDocument79 paginiARDS With Pathophysiologymabec pagaduan95% (19)
- Diabetic Ketoacidosis Case PresentationDocument37 paginiDiabetic Ketoacidosis Case PresentationNathan Vince Cruz100% (2)
- DKADocument64 paginiDKAAravindhan Gunasekaran PaediatricianÎncă nu există evaluări
- DkaDocument83 paginiDkaRajaKumar Ponnana100% (1)
- Emergency Nursing Nclex ExamDocument19 paginiEmergency Nursing Nclex ExamsjardioÎncă nu există evaluări
- Diabetic KetoacidosisDocument6 paginiDiabetic KetoacidosisRain Catan Gagarra Saquin100% (1)
- Diabetic Ketoacidosis Case StudyDocument5 paginiDiabetic Ketoacidosis Case Studyjc_albano29100% (7)
- Diabetes MellitusDocument9 paginiDiabetes MellitusM. Joyce100% (2)
- Liver CirrhosisDocument31 paginiLiver CirrhosisMarisol Jane Jomaya50% (2)
- Sensation and Perception HandoutsDocument3 paginiSensation and Perception HandoutsMariaMirandaJrÎncă nu există evaluări
- Diabetic KetoacidosisDocument76 paginiDiabetic Ketoacidosisniyigok100% (1)
- Diabetic Ketoacidosis (DKA)Document33 paginiDiabetic Ketoacidosis (DKA)Eric Chye Teck100% (1)
- Slave Breakers 2Document167 paginiSlave Breakers 2kjmama100% (1)
- Nursing Care Plan For "Diabetes Mellitus - Diabetic Ketoacidosis"Document17 paginiNursing Care Plan For "Diabetes Mellitus - Diabetic Ketoacidosis"jhonroks97% (36)
- Heart FailureDocument94 paginiHeart FailureAnusha Verghese100% (1)
- Myocardial InfarctionDocument28 paginiMyocardial Infarctionshaitabligan100% (1)
- Pulmonary EdemaDocument59 paginiPulmonary EdemamaibejoseÎncă nu există evaluări
- Diabetic Ketoacidosis Case StudyDocument6 paginiDiabetic Ketoacidosis Case StudyHomework Ping100% (2)
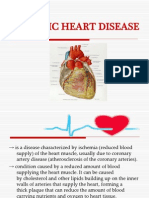
- Ischemic Heart Disease PWDocument13 paginiIschemic Heart Disease PWEunica RamosÎncă nu există evaluări
- Pulmonary EmbolismDocument14 paginiPulmonary EmbolismMutaz Dredei100% (5)
- DKA ManagementDocument59 paginiDKA Managementnatalieshirley100% (1)
- Diabetic KetoacidosisDocument39 paginiDiabetic KetoacidosisNathasya B.W.Încă nu există evaluări
- Patofisiologi Shock CardiogenicDocument44 paginiPatofisiologi Shock CardiogenicGalih Arief Harimurti Wawolumaja100% (1)
- Cardiogenic ShockDocument21 paginiCardiogenic ShockIslamOteshÎncă nu există evaluări
- DKA (Diabetic Ketoacidosis)Document3 paginiDKA (Diabetic Ketoacidosis)Hassan.shehri83% (6)
- Endocrine Pathophysiology Nursing Notes - Part 2Document10 paginiEndocrine Pathophysiology Nursing Notes - Part 2grad_nurse_2015100% (1)
- Diabetic KetoacidosisDocument41 paginiDiabetic KetoacidosisdenekeÎncă nu există evaluări
- APN2 Case Study - DKADocument25 paginiAPN2 Case Study - DKAElizabeth Ho100% (4)
- Diabetic Ketoacidosis (Dka)Document18 paginiDiabetic Ketoacidosis (Dka)dr.Bobi Ahmad Sahid, S.Kep100% (2)
- GI Bleeding - NursesDocument71 paginiGI Bleeding - Nursesapi-3760283100% (6)
- Diabetic KetoacidosisDocument5 paginiDiabetic KetoacidosisJill Catherine Cabana100% (3)
- Pulmonary EmbolismDocument5 paginiPulmonary EmbolismNica Duco100% (2)
- Case Study: Diabetic KetoacidosisDocument66 paginiCase Study: Diabetic Ketoacidosisllaychin100% (2)
- Myocardial InfarctionDocument40 paginiMyocardial InfarctionHIRANGER100% (3)
- Cardiogenic ShockDocument2 paginiCardiogenic ShockChristine QuironaÎncă nu există evaluări
- From Li ZhongziDocument4 paginiFrom Li ZhongziRadhakrishnan KasthuriÎncă nu există evaluări
- Clinical Practice Guidelines: Management of Type 2 Diabetes Mellitus (5 Edition) 2015Document13 paginiClinical Practice Guidelines: Management of Type 2 Diabetes Mellitus (5 Edition) 2015Azim Abd Razak100% (1)
- CABGDocument32 paginiCABGأمينةأحمد100% (1)
- Assignment Module 3Document14 paginiAssignment Module 3Asshi Sha50% (4)
- CopdDocument60 paginiCopdRizqy Shofianingrum100% (1)
- Patent Ductus Arteriosus: by Dr. Hanan Zekri Khaled Lecturer of Pediatrics Pediatric CardiologyDocument36 paginiPatent Ductus Arteriosus: by Dr. Hanan Zekri Khaled Lecturer of Pediatrics Pediatric CardiologyEira RajkumarÎncă nu există evaluări
- Diabetic KetoacidosisDocument3 paginiDiabetic KetoacidosisJanna FavilaÎncă nu există evaluări
- Diabetic Ketoacidosis PathwayDocument22 paginiDiabetic Ketoacidosis PathwaySri Nath100% (1)
- Diabetic KetoacidosisDocument38 paginiDiabetic KetoacidosisAwatef AbushhiwaÎncă nu există evaluări
- Pulmonary EmbolismDocument80 paginiPulmonary EmbolismVarun B Renukappa100% (1)
- Case Study PresentationDocument44 paginiCase Study Presentationapi-31876231450% (2)
- Diabetic KetoacidosisDocument22 paginiDiabetic KetoacidosismartinÎncă nu există evaluări
- Diabetic Ketoacidosis: Presented by The Students From Roll Numbers 31 - 40Document20 paginiDiabetic Ketoacidosis: Presented by The Students From Roll Numbers 31 - 40HUSSAIN NAZEESHAÎncă nu există evaluări
- Chronic Renal FailureDocument37 paginiChronic Renal Failuredorkiebaby100% (10)
- Upper and Lower Gastrointestinal BleedingDocument36 paginiUpper and Lower Gastrointestinal BleedingDr. Shatdal Chaudhary100% (2)
- Angina PectorisDocument17 paginiAngina PectorisRacel HernandezÎncă nu există evaluări
- HypokalemiaDocument3 paginiHypokalemiaSergeiÎncă nu există evaluări
- Diabetic Ketoacidosis Acute Management: A State of Absolute Insulin BankruptcyDocument24 paginiDiabetic Ketoacidosis Acute Management: A State of Absolute Insulin BankruptcyGwEn LimÎncă nu există evaluări
- HypertensionDocument8 paginiHypertensiongilma100% (3)
- Diabetes Mellitus Complications: Ssenabulya F Ronny MBCHB V Moderator Dr. Mutebi 4B Endocrinology UnitDocument55 paginiDiabetes Mellitus Complications: Ssenabulya F Ronny MBCHB V Moderator Dr. Mutebi 4B Endocrinology UnitNinaÎncă nu există evaluări
- Diabetic KetoacidosisDocument10 paginiDiabetic Ketoacidosisagar agarÎncă nu există evaluări
- Acute Metabolic Complications of Diabetes MellitusDocument54 paginiAcute Metabolic Complications of Diabetes MellitusPrincewill SeiyefaÎncă nu există evaluări
- 128 Diabetic KetoacidosisDocument9 pagini128 Diabetic KetoacidosisDite Bayu NugrohoÎncă nu există evaluări
- PhysioEx Exercise 9 Activity 5Document3 paginiPhysioEx Exercise 9 Activity 5Gonzeilo11Încă nu există evaluări
- Kreisberg-Zakarin Et Al IPNS Antonie Van Leeuwenhoek 1999Document8 paginiKreisberg-Zakarin Et Al IPNS Antonie Van Leeuwenhoek 1999ElÎncă nu există evaluări
- The Independence of Combinatory Semantic Processing: Evidence From Event-Related PotentialsDocument21 paginiThe Independence of Combinatory Semantic Processing: Evidence From Event-Related Potentialsdkm2030Încă nu există evaluări
- 8 Benefits of Warming UpDocument2 pagini8 Benefits of Warming UpJevyn KhoÎncă nu există evaluări
- Nano DentistryDocument6 paginiNano DentistryanugrasÎncă nu există evaluări
- ControlDocument12 paginiControlSirVietaÎncă nu există evaluări
- Human Anatomy 4th Edition McKinley Test Bank 1Document35 paginiHuman Anatomy 4th Edition McKinley Test Bank 1donnawugnwsjrzcxt100% (27)
- BMJ - Hypovolemic ShockDocument5 paginiBMJ - Hypovolemic ShockSamer Darwiche Yasiin100% (1)
- Guide To AMA Manual of StyleDocument5 paginiGuide To AMA Manual of StyleAbo Ahmed TarekÎncă nu există evaluări
- Principles of Endocrinology Szathmari Miklos 2010Document25 paginiPrinciples of Endocrinology Szathmari Miklos 2010Ryan James Lorenzo MiguelÎncă nu există evaluări
- تقرير ثرموداينمكDocument5 paginiتقرير ثرموداينمكاحمد كاظمÎncă nu există evaluări
- Biological (Met)Document52 paginiBiological (Met)SirLhitz B. UmaliÎncă nu există evaluări
- Neonatal PneumoniaDocument2 paginiNeonatal PneumoniaJustin EduardoÎncă nu există evaluări
- Dewey: DecimalDocument888 paginiDewey: Decimalpratiik pyakurelÎncă nu există evaluări
- Agriculture& Horticulture Conference BrochureDocument6 paginiAgriculture& Horticulture Conference BrochureAgriculture conferenceÎncă nu există evaluări
- Muscarinic Jones Concert: Skeletal Muscle Contraction Analogy WorksheetDocument5 paginiMuscarinic Jones Concert: Skeletal Muscle Contraction Analogy WorksheetCharles VollmersÎncă nu există evaluări
- Class XI Practicals Term2Document5 paginiClass XI Practicals Term2Prince KÎncă nu există evaluări
- BrodmannDocument2 paginiBrodmannEdelleMojicaDafilmotoÎncă nu există evaluări
- Irregular PluralsDocument19 paginiIrregular PluralsDj-mauro Mulchen ChileÎncă nu există evaluări
- 1 Il-10 ElisaDocument15 pagini1 Il-10 ElisaYousra ZeidanÎncă nu există evaluări
- 70037Document4 pagini70037Nabila SaribanunÎncă nu există evaluări
- SRIVASTAVA & SINGH, 2008 - Brissid Echinoid Eupatagus From The Khuiala Formation, Jaisalmer District, Rajasthan, IndiaDocument6 paginiSRIVASTAVA & SINGH, 2008 - Brissid Echinoid Eupatagus From The Khuiala Formation, Jaisalmer District, Rajasthan, Indiachindas4321Încă nu există evaluări